Dr Nigel Hacking, is a senior Interventional Radiologist and leading expert in prostate artery embolisation (PAE). Dr Hacking has pioneered this minimally invasive and non-surgical option for treating the symptoms of enlarged prostate / lower urinary tract symptoms (LUTS). Dr Nigel Hacking is the acknowledged expert in the UK. The article explains what is involved in this highly promising and now fully recognised new treatment for benign prostatic hyperplasia (BPH) called Prostate Artery Embolisation (PAE).
This new therapy will be of particular interest to men who are experiencing LUTS as well as those who have previously received medical or even surgical treatment for this condition that has not proved successful.
Contents - Prostate Artery Embolisation for BPH
- Introduction to benign prostatic hyperplasia
- Symptoms of BPH
- Treatment of BPH
- Trans Arterial Embolisation
- Prostate Artery Embolisation
Introduction to benign prostatic hyperplasia
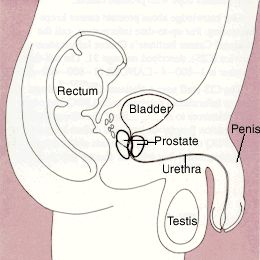
Benign prostatic hyperplasia (BPH - also called benign prostate enlargement) is the condition that occurs when the prostate gland increases in size without there being any malignant cause. As the prostate enlarges it leads to compression and then obstruction of the urethra, which in turn affects urinary flow. The symptoms include urinary frequency, urinary urgency, hesitancy in urination, poor stream and incomplete bladder emptying. Partial obstruction can ultimately become complete causing acute urinary retention and the urgent requirement for a bladder catheter. BPH is not however a pre-malignant condition. BPH becomes increasingly common with age and has an impact on the quality of life for a considerable number of men aged over fifty years.
The process by which the prostate begins enlarging starts around the age of 30 and up to 50% of men will show histological signs (changes within the tissues) of BPH by 50 years of age. By 80 years of age this rises to 75% although not all of these men will have symptoms. Symptomatic BPH occurs in up to 50% of men of middle age or older.
Traditionally, BPH has been managed with lifestyle changes and medication in the first instance but if the symptoms progress or become severe then surgery may be required. However, as this is an age-related condition fitness and suitability for surgery is often an issue.
Symptoms of BPH
The symptoms of BPH fall into two broad categories
- Voiding (weak stream, hesitancy, stop and start micturition)
- Storage (frequency, urgency, nocturia, leaking)
Treatment of BPH
Both of the sets of symptoms listed above occur in BPH. The management of BPH varies according to the nature and severity of the symptoms. Lifestyle changes and medication (such as the drugs known as alpha blockers and 5ɑ-reductase inhibitors) are used initially, but if the symptoms progress despite conservative therapy then surgery may well be suggested.
There are a number of different forms of surgery that will typically be offered depending on the size of the prostate gland including Trans Urethral Prostatectomy (TURP) or Open Prostatectomy. However, minimally invasive thermal ablation using microwave energy (TUMT), radiofrequency (RF) and laser energy (PVP, HoLAP/HoLEP) have not gained widespread usage.
Trans Arterial Embolisation
Trans-arterial embolisation is a non-surgical, minimally invasive procedure, that has been used in many clinical settings. The procedure involves reducing or blocking blood flow by injecting tiny particles into blood vessels.
Initially introduced to stem life-threatening haemorrhage it is now used to block the blood vessels that serve tumours prior to surgery and also for definitive palliative treatment of tumours. It has been used in the setting of prostatic disease for many years either to stem acute or chronic bleeding due to advanced prostatic cancer, but also to control bleeding after prostatic surgery.
Prostate Artery Embolisation
Over the last decade prostate artery embolisation (PAE) has been the subject of two clinical studies, one in Sao Paulo, Brazil the another in Lisbon, Portugal. The study groups have been testing the hypothesis that trans-arterial embolisation of the prostate could lead to the death of the blood-rich and overgrown prostatic tissue, which in turn would result in a subsequent reduction in obstructive urinary symptoms. Presentations to the International Interventional Radiology conferences during 2010, 2011 and 2012 confirmed the initial optimism in over 400 cases. In February 2013 the Portuguese group published initial and mid term results on over 250 men. Clinical improvement was seen in around 80% at 6-12 months and still over 70% at 3 year follow up.
Procedure for BPH
The procedure is performed by trained Interventional Radiologists who are experienced in advanced embolisation techniques. It involves a groin puncture and then thin, hollow tubes known as catheters, are placed into both right and left prostatic arteries. These are then closed using 100-200 micron-sized embolic particles. The procedure takes approximately one to two hours to perform and the patient can be discharged after 4–6 hours provided he is fit. Men needing to travel out of the area or those who are less fit will require an overnight stay in hospital.
Post-procedural pain is usually minor. Complications reported to date have been rare and mostly involve minor bruising of the groin. Three cases of non-target embolisation of the bladder and rectum have been reported out of over 400 cases; of these, one required surgical bladder repair. It is encouraging that the common side effects of TURP, such as transient incontinence, erectile dysfunction and particularly retrograde ejaculation have not been reported and improvement or relief of symptoms has been reported in 80% of patients with up to a one year follow-up.
In light of these results, a carefully Monitored Clinical Introduction in 20 men with proven and symptomatic BPH, that had not responded to medical treatment was instigated at Southampton University Hospitals in 2012. The procedure was technically successful in all 20 patients enrolled and clinical improvement, although modest in some, was been seen in 90%. There were no serious complications and post procedural pain was mild to moderate only. In all but exceptional cases the procedures were performed as a day-case.
The first UK medical symposium on Prostate Artery Embolisation was held at the TEAM-UK 2012 meeting in Birmingham. Initial results from the Southampton series were presented at the British Society of Interventional Radiologists in November 2012.
What patients are saying about PAE
Please read article, Prostate artery embolisation - the patient's view written for the benefit of other patients.
I did not need the analgesics, and noticed an improvement in urination in the first week
A GP referral for treatment
A GP or urology referral will be required and a full assessment with both a urologist and a radiologist will be required before PAE can be offered. Please click the Dr Hacking's contact button.
Editors note:
Further clinical studies have taken place in the United Kingdom on the effectiveness of PAE for relieving the symptoms of BPH since the publication of this article - to find out more see Promising results treating Benign Prostatic Hyperplasia (BPH) by PAE
Or, for further information on the author of this article, Consultant Radiologist, Dr Nigel Hacking, please click here.
Inability to maintain a penile erection for sexual intercourse, also referred to as impotence.
Full medical glossary








