Laparoscopic Radical Prostatectomy - Contents
- What is laparoscopic radical prostatectomy?
- Pre-operative staging
- What are the advantages of prostate keyhole surgery?
- What are the risks of having a laparoscopic radical prostatectomy?
- Is there a cut-off age for surgery?
- What happens after the operation?
- Case study
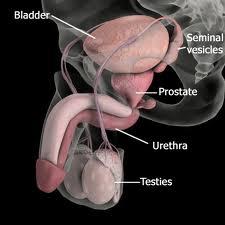
What is laparoscopic radical prostatectomy?
Laparoscopic radical prostatectomy, also known as keyhole prostatectomy, is a minimally invasive operation performed by a Urological Surgeon to treat, and cure, prostate cancer. It is performed under general anaesthetic and involves removing the entire prostate gland, seminal vesicles, and sometimes the lymph glands within the pelvis. The bladder is then re-attached to the urethra with sutures.
Laparoscopic radical prostatectomy is endorsed by the National Institute for Health and Clinical Excellence (NICE).
Pre-operative staging
Laparoscopic radical prostatectomy can only be performed on prostate-confined prostate cancer and as such, an MRI scan of the prostate will be taken, sometimes along with a prostate biopsy, to establish if the patient has organ-confined disease or not. A modern type of MRI known as a diffusion weighted MRI can show up small cancers that may not have been found during the biopsy and these can therefore help to plan surgery in finer detail.
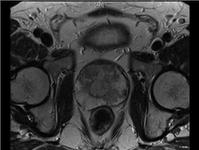
The prostate is analysed by a pathologist giving a precise understanding of the amount and type of cancer removed, and whether any additional treatments such as prostatic bed radiotherapy will be required.
In low risk disease, a decision can be made to spare the nerves in an attempt to preserve potency, although in a high risk disease a wide local excision will normally be performed.
What are the advantages of keyhole surgery?
- Less complications both during, and after, the operation e.g. damage to adjacent structures such as bowel and major blood vessels.
- Better cancer control with less residual tumour and need for adjuvant radiotherapy following surgery.
- Shorter hospital stay; most patients are discharged after one or two nights in hospital.
- Less blood loss; blood transfusions are very rare and occur in less than 1% of patients.
- Less post-operative pain and a quicker return to normal activities. The smaller incisions, no larger than 2–3cm, result in less pain and only simple analgesics such as paracetamol and diclofenac are needed following surgery. It is very rare to require morphine-based analgesia resulting in fewer side effects such as drowsiness and constipation.
What are the differences between keyhole surgery and daVinci?
Laparoscopic radical prostatectomy is a minimally invasive operation for localised prostate cancer, the daVinci is a robotic tool used by the surgeon to perform this operation. The outcomes are equivocal in terms of cancer and functional outcomes such as continence and potency.
Should any other options be considered?
The laparoscopic radical prostatectomy operation is for localised prostate cancer, other options such as brachytherapy or external beam radiation exist. There are pros and cons to each of the treatments and a discussion between the patient and their consultant should occur to decide which way to go, this is a complex decision with many different options.
What are the risks of having a laparoscopic radical prostatectomy?
General risks of having any operation
- An infection of the wound, chest or urinary tract. Antibiotics are given during the operation but not afterwards as these can lead to side effects, drug resistant strains of viruses, and to minimise side effects, resistance and problems such as Clostridium difficile which can occur when the bacteria in the gut are wiped out due to antibiotics and can lead to diarrhoea and intestinal disease.
- Bleeding, during or after the operation. Laparoscopic procedures lead to much less bleeding however, due to better vision and the use of state of the art vascular sealants.
- Thrombosis in the form of Deep Vein Thrombosis (DVT) or pulmonary embolism. To reduce this risk, patients self-administer anti-thrombotic agents with a needle for 40 days after the procedure.
Specific risks of having a laparoscopic radical prostatectomy
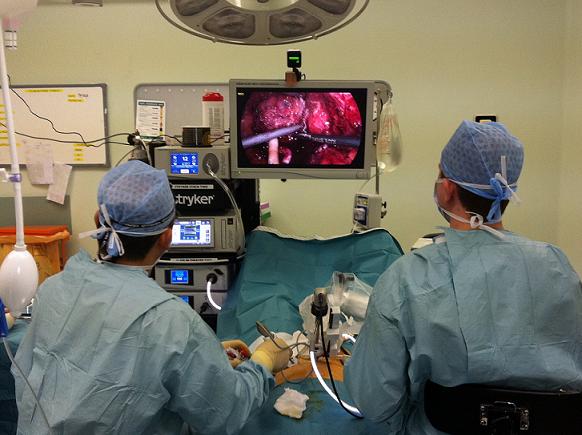
- Urinary incontinence. All men will suffer unintentional leakage of urine when the catheter is removed one week after the operation and pads are necessary. Patients are taught to perform pelvic floor to help regain continence; this can take days, weeks or months depending on the patient. In the long term, keyhole prostate surgery gives improved continence outcomes compared to traditional open surgery.
- Erectile dysfunction. Depending on the amount and type of cancer it may be possible to attempt to protect or spare nerves and blood vessels that are involved in erections however this does not guarantee future erections and recovery can take up to two years. Men who have existing erectile problems will see a further decline and are the most difficult to treat. Men wishing to return to potency after the operation are encouraged to engage in penile rehabilitation. This may involve the use of daily tablets such as tadafil or sildenafil citrate and penile vacuum pumps.
- Bladder neck contracture; a narrowing of the connection between the bladder and urethra due to excessive scar tissue, this can lead to symptoms such as incontinence. The connection between the bladder and urethra will occasionally need to be released under anaesthetic as a day case.
- Rectal injury. This is a rare (<1%) but serious complication and may require a temporary colostomy.
Is there a cut-off age for surgery?
There has been quite a change in this area in recent years. Traditionally, a cut-off at 70 years for surgery used to be applied but not any more. A patient's physiological age rather than chronological age is considered. We live in an age of 'pateint choice' and most surgeons would not deny a fit 75 year old who wanted surgery. Minimally invisive surgery is much better tolerated than traditional open surgery in the older man and length of stay and recovery is comparable with younger men (this is not the case with open surgery).
What happens after the operation?
Patients are encouraged to eat and drink normally on the night of the operation and most patients will be discharged one or two nights after the operation with a catheter to be removed after a week. Some abdominal bloating is expected and bowels will typically open after 2–3 days. Drinking plenty of water (two to three pints a day) is essential to ensure a good urine output and prevent catheter blockages.
Any activity more than light walking i.e. driving, lifting and gardening, should be avoided for two to three weeks after the operation to prevent damage to internal healing.
The oncological result is monitored using PSA tests, with the first test taken at 4–6 weeks after the surgery.
Case study
Mr G, a fit and well 56 year old, was getting up at night to urinate and went to see his GP. He thought it was related to late nights at work and stress but was seeking reassurance. After a thorough review from his GP his PSA level was found to be high at 8.5µg/L (a normal level is below 3.0µg/L).
He was reviewed urologically and by this time his urinary symptoms had improved. A palpable nodule was felt during a rectal examination and a prostate biopsy was undertaken.
MRI staging was undertaken and prostate-confined disease was confirmed. Due to having intermediate risk disease, cancer treatment was recommended as opposed to active surveillance. Mr G was then seen in a joint consultation by a surgical urologist and a radiation oncologist to decide on his treatment; either a laparoscopic radical prostatectomy or radical radiotherapy and two years of hormone ablation therapy (medical castration).
Mr G discussed his options with his family and GP and decided to take the surgical route. The multidisciplinary team had recommended surgery due to the age of Mr G as surgery is usually recommended to the younger, fitter patients.
After admission, the operation proceeded uneventfully and he was discharged home the following day with a catheter. The pain was very minimal requiring only simple analgesia. After the catheter was removed he was incontinent for the first three weeks requiring pad changes every 3–4 hours but by week four he was in full control, only leaking when lifting or stooping. By week four he was back playing golf and was able to work from home after just one week. Six months following surgery his disease is in remission with an un-recordable PSA. He has full control of his bladder but can only achieve a partial erection with an oral phosphodiesterase inhibitor but things are slowly improving. Full potency recovery is possible over the next 18 months.








