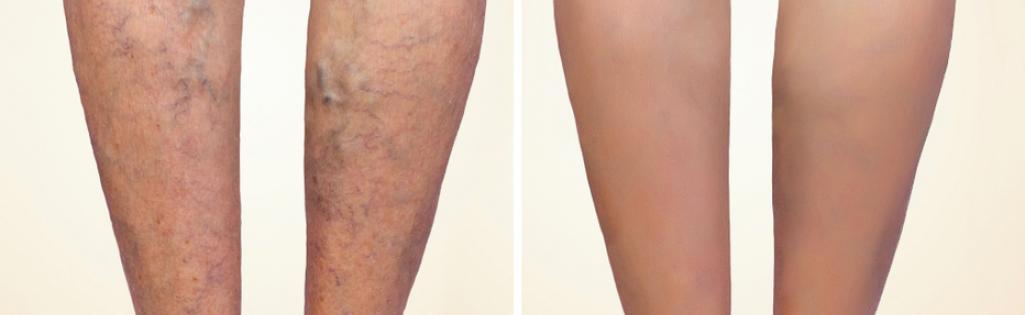
The appearance of veins on our legs, no matter how small, is a clear indication of the potential progression of vein disease and should therefore be taken seriously. Veins usually carry blood from the legs up to the heart. The blood is prevented from flowing backwards by one-way valves, however, if these valves become faulty blood is able to flow back down into the legs where it pools and hardens causing varicose veins.
Contents
- Symptoms and assessment of varicose veins
- Ultrasound ‘duplex’ scan
- Treating varicose veins with thermal treatment ablation
- The laser or radiofrequency ablation debate
- Non thermal treatments for varicose veins
- Treating varicose veins with Avulsion (micro-phlebectomy)
- Moving on from the past
- The results of varicose vein treatment
Symptoms differ in men and women
 Varicose vein symptoms affect men and women differently. In men, itching of the skin is the main symptom whilst women typically report heaviness and aching. However, anyone can have any combination of these symptoms. It is worth noting also that many of these symptoms are not specific to varicose veins only – for example pain may be due to arthritis.
Varicose vein symptoms affect men and women differently. In men, itching of the skin is the main symptom whilst women typically report heaviness and aching. However, anyone can have any combination of these symptoms. It is worth noting also that many of these symptoms are not specific to varicose veins only – for example pain may be due to arthritis.
How are varicose veins assessed?
A world class care pathway starts with a comprehensive history and 'Aberdeen' questionnaire, which looks at the presentation of symptoms and how they affect our daily lives. This assessment is followed by a detailed investigation using a duplex scanner. In some cases, a patient will also be referred for an MRI scan in order to identify problems above the groin area in the abdomen and pelvis. A reason for scanning the pelvis and abdomen may be early, aggressive recurrence of varicosities, a predominantly left sided problem or if you have had deep vein thrombosis (DVT). A severe leg ulcer that hasn’t responded to treatment may also need an MRI scan. Syndromes such as May-Thurner syndrome or pelvic congestion syndrome can be identified in this way.
Ultrasound ‘duplex’ scan
The introduction of vascular ultrasound (a duplex scan) has been a game changer for patients in terms of the quality of treatment they can expect to receive. Visible varicose veins are just the tip of the iceberg; the ultrasound scan looks at everything else. Improvements in diagnostic assessment have been central to explaining why traditional surgery did not provide consistent results. The surgeon simply didn’t have a sufficiently accurate map or any way of knowing that all the necessary vein had been removed.
Ultrasound provides that detailed map of the venous system, specifically the size and location of problems in the veins. The scan also confirms the health of the deep vein system. This is important because if there is a blockage or damage in the deep veins it may alter treatment plans for the superficial veins.
The scan also helps to manage expectations as to the likely symptomatic and cosmetic success from treating the superficial veins. If reflux is present in the deep veins, we may still be able to treat the superficial veins, but the symptomatic improvement and cosmetic results may not be as good. It is important to remember that the scan is not to confirm the presence of varicose veins, but to understand how these smaller veins are fed by failures in the bigger, deeper veins.
Modern treatments are divided broadly into thermal (those that use heat) and non-thermal (those that use chemicals like sclerosants and glue), All treatments, thermal or non-thermal are minimally invasive, which means faster recovery, lower complication and recurrence rates compared to the traditional (and now largely outdated) method of stripping.
Treating varicose veins with thermal treatment ablation
Usually under local anaesthetic, a probe is inserted into and along the vein. As the probe is pulled back along the vein, thermal energy is applied to cause the blood to clot and the vein fibroses, effectively blocking it to any further blood flow.
The treatment requires the consistent delivery of energy along the vein as the probe is pulled back. Too much energy and you burn the vein, too fast (or too little), and you don’t successfully treat the vein.
The laser or radiofrequency ablation debate
Both methods of applying thermal energy to the affected areas work effectively. The contention is over the way in which laser delivers energy, relying on surgeon accuracy in contrast to the systematic capability of radiofrequency ablation. This factor opens up the potential for variability in the outcomes a surgeon can predictably deliver over time. For example, if a surgeon wants to treat a 10cm section of vein, delivering 80 joules per centimetre the surgeon will manually pull back the catheter, guided by a metronomic bleeping sound that is emitted. After 10cm the surgeon will try ensure that a total of 800 joules has been delivered giving an average of 80J/cm but that may not have been delivered as precisely to each centimetre of the vein; sometimes starting too fast and slowing toward the end or vice versa. This variation is predominantly caused by human factors, tiredness at the end of the list, a bad day, surgeon experience or just the list running behind and it’s the 10th patient of the day. .
Radio frequency on the other hand is a staged treatment in which the surgeon treats segments at a time rather than continuous pull back. This means the delivery of energy is more consistent and in addition the machine gives feedback as to how well the treatment is working indirectly via the measurement of how much energy is required to heat the vein to the treatment temperature. This generally means that treatment using Radiofrequency is more consistent and ensures more predictable results. From a patient perspective, there is evidence that radio frequency is less painful for the patient following treatment.
Non thermal treatments for varicose veins
 The primary non-thermal treatment for varicose veins is foam sclerotherapy, based on the Tessari technique, invented in France. A small amount of sclerosant is mixed with air to create foam which is injected into the vein. The foam pushes the sclerosant into contact with the vein wall displacing blood. The chemicals damage the vein wall, causing it to “block off” the vein.
The primary non-thermal treatment for varicose veins is foam sclerotherapy, based on the Tessari technique, invented in France. A small amount of sclerosant is mixed with air to create foam which is injected into the vein. The foam pushes the sclerosant into contact with the vein wall displacing blood. The chemicals damage the vein wall, causing it to “block off” the vein.
Complications with foam treatment are rare. If a patient has a predisposition towards migraine then the chemicals in the foam can bring this on. Also, occasionally some patients experience temporary and minor visual impairment.
This treatment is effective for tidying up small veins, but data suggests it is less effective than radiofrequency ablation, which is why we don’t use it for everything. Foam sclerotherapy comes in a range of concentrations and the surgeon will not know which concentration will deliver the best results, so will start at 0.5%, using stronger formulas in follow-up sessions if required. There is a limit to the amount of foam the body can accommodate so typically foam treatment is completed over a series of visits. Using too high a concentration can lead to staining on the skin, so it’s important to start with lower concentrations of foam.
There are additional techniques that combine the use of sclerosant with a catheter that enhances the efficacy of the sclerosant (Clarivein or MOCA) and also the use of glues that stick the vein shut. These techniques all have the advantage of not needing an infusion of the local anaesthetic tumescence but appear to (for MOCA) have slightly higher rates of recurrence and in the case of glue reported issues with allergic reactions.
Treating varicose veins with Avulsion (micro-phlebectomy)
This is a surgical process, that can be performed under local anaesthetic, requiring a number of incisions along the leg. At each incision, the surgeon will remove a small proportion of the vein. After the procedure, small cuts along the leg that require simple dressings that heal well with time.
This practice is effective for larger veins. If, however you treat the larger veins with ablation first, in around 70% of cases the remaining veins will get better by themselves and avulsions are not required.
Moving on from the past
Whilst there is still a reasonable amount of vein stripping occurring in the NHS, this really shouldn’t be the preferred method for treating varicose veins. Indeed, for recurrent varicose veins, the latest guidelines from international societies and organisations such as NICE suggest that other methods of treatment, especially for recurrent veins, should be prioritised.
Overall, this procedure carries with it a 1% chance of serious complication, such as DVT, pulmonary embolism (blood clot in the lungs) or neurovascular damage. There is also a 15% chance of minor complications such as infections, seroma (build-up of fluid under the skin), nerve damage or bleeding. The surgery also requires general anaesthetic and results in prolonged recovery 7/14 days to drive, and 14/21 days off work.
Actually, the process can appear to be quite brutal and when not guided by ultrasound, the surgeon would have no way of knowing if the entire vein had been removed. This is why outcomes are so poor with 26% of patients complaining their veins were no better after surgery. Overall, 34% of patients will not be happy with the outcome.
The results of varicose vein treatment
It is a common saying among vascular surgeons that after surgery a patient’s eyesight gets better, whilst the memory fades. This is because people typically only “see” the bigger varicosities prior to treatment. Once treated, the smaller veins come into sight. This is why the process is designed in three stages as follows:
- scan,
- treatment and
- follow-up.
At the follow-up, minor flare veins can be treated with foam to improve the overall cosmetic effect. Patients need to be patient and trust the process, which has proven to deliver excellent outcomes.
In summary
In summary, modern minimally invasive techniques facilitate a quick recovery, address a range of symptoms and produce exceptional cosmetic results.