Balloon Kyphoplasty is a relatively new technique for treating vertebral/spinal fractures. This article will be of interest to those seeking an alternative treatment to the traditional medicinal or orthopaedic methods.
Contents
- Introduction
- How common are spine fractures (VCF's)?
- Consequences of VCFs
- Treatment goals
- Minimally invasive treatment
- Results
- Spinal deformity correction
- Pain relief
- Early remobilisation
- Quality of life
- Summary
Introduction
Spinal fractures are often the result of bone weakening (osteoporosis) and are known as vertebral body fractures. These fractures are a serious problem and have a highly negative impact on quality of life through pain and reduced mobility. More conservative methods of treatment aim simply at pain reduction and this often requires narcotic pain medication, bed rest and/or spinal orthotic support. Satisfactory pain control is often only achieved after several weeks of treatment. On the other hand, percutaneous ("keyhole") injection of bone cement into the fractured spine vertebra has been proven to be a therapeutic option that results in rapid pain relief. One of the most recent developments of this form of treatment is Balloon Kyphoplasty (BKP). There are additional advantages associated with BKP, the procedure enables the correction of local spinal deformity, this improves overall spinal alignment and therefore reduces the risk of lung complications and recurrent fractures. Following a number of years experience in practical application, BKP has been proven to be a very safe technique.
How common are spine fractures (VCF's)?
Osteoporosis can affect all parts of the skeleton and the disease causes a reduction in bone mineral density (BMD), the microarchitecture is disrupted, and the amount and variety of non-collagenous proteins is altered. Therefore osteoporotic bones are at an increased risk of fractures. These fractures typically occur in women after the menopause, because oestrogen assists in maintaining good bone strength. As oestrogen levels decline, bone is resorped or lost. Osteoporosis can also occur in men. Other risk factors include delayed puberty, poor calcium intake, smoking, excess alcohol consumption or use of certain medications such as glucocorticoid steroids in the treatment of specific diseases such as rheumatic disorders.
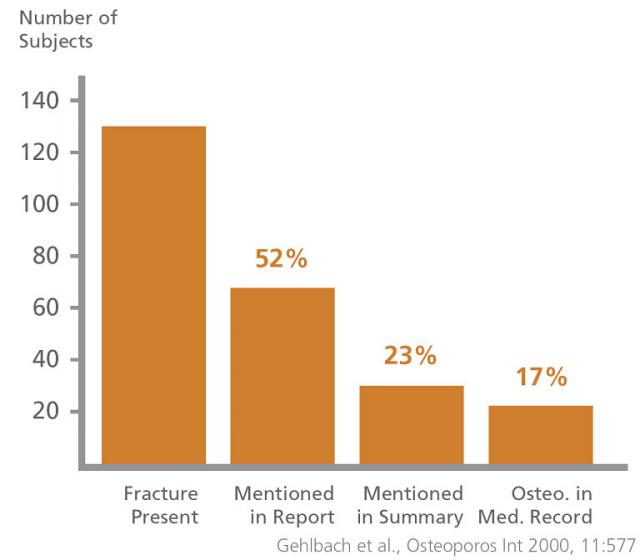
As bones weaken, they are more likely to fracture. Osteoporotic fractures commonly affect the hip, wrist and spine. According to the International Osteoporosis Foundation, 40% of all middle-aged women (8 out of 20) and 15% of middle-aged men (3 out of 20) in Europe will suffer one or more osteoporotic fractures during their remaining lifetime. In fact, at any time point in Europe, there will be a fracture every 30 seconds as a consequence of osteoporosis. Furthermore, the estimated number of patients with osteoporosis will double over the next 50 years in line with the projected increase in the aging population and as a result of poor lifestyle factors. However, despite increasing incidence of osteoporotic fractures, the scale of problem continues to be seriously under-recognised with only 50% of osteoporotic vertebral compression fractures (VCFs) being correctly diagnosed (Fig.1)
Consequences of VCFs
VCFs that are secondary to osteoporosis can occur spontaneously or after minor trauma. VCFs cause the spine to shorten and result in a misalignment or "kyphotic spinal deformity". As the centre of gravity shifts forwards, a larger bending moment is created. The posterior muscles and ligaments must counterbalance this increased bending, so that the osteoporotic anterior spine is forced to withstand larger compressive stresses.
Over time, an untreated spinal fracture heals in a deformed state or "hyperkyphosis", which serves to preserve the altered biomechanics. Whether painful or not, the long term consequences of VCFs can be devastating. As a result of the altered biomechanics of the spine, the knees bend and the pelvis tilts forward to counteract the forward bending or "positive sagittal balance". This creates a change in balance, a decrease in walking speed (gait velocity) and increased muscle fatigue which in-turn leads to an increased risk of falls and subsequent fractures.
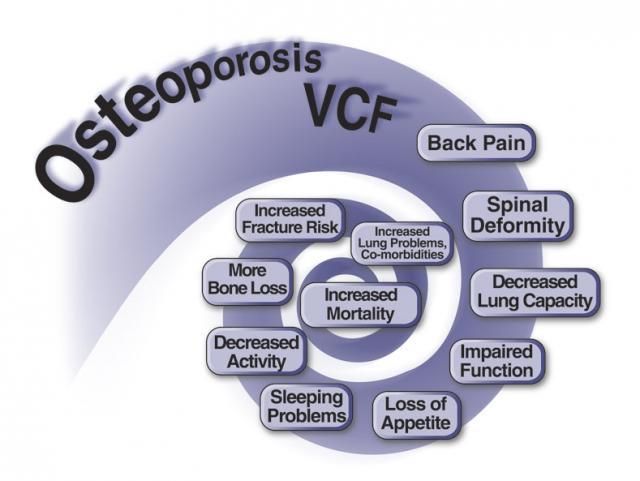
This often leads to:
- Impaired function and decreased quality of life
- An increased risk of subsequent fractures
- Impaired pulmonary function and increased lung disorders
- Sleep disorders
- A compressed stomach leading to a decreased appetite, potentially resulting in malnutrition
- 23-34% increased mortality compared to patients without VCF
Treatment goals
There are four basic medical principles for the management of fractures.
- Fracture reduction and fixation to restore anatomical relationships
- Stability by fixation or splintage, depending on the nature of fracture characteristics and injury requirements
- Preservation of blood supply to soft tissues and bone by careful handling and gentle reduction techniques
- Early and safe mobilisation of the fracture and patient.
For vertebral compression fractures this means that historically, it was only possible to apply these basic principles to traumatic vertebral compression fractures. Such reductions in individuals with normal bone were often treated with open reduction, internal fixation and fusion techniques. These techniques are typically difficult to perform and have inferior outcomes when dealing with low quality and soft osteoporotic bone.
Until recently, the collapse of osteoporotic vertebral bodies was treated non-operatively with conservative treatments which included bed rest, back braces and pain medications. These methods allowed the bone to heal in a suboptimal or deformed state and de facto, did not fulfill the fundamental orthopaedic principles of fracture management.
Minimally invasive treatment
At the start of 1998 a new, minimally invasive procedure called 'Balloon Kyphoplasty' became available, which addresses the problem of painful vertebral compression fractures. BKP is a minimally invasive surgical procedure used to treat patients with one or more VCFs caused by osteoporosis (primary or secondary) or osteolytic lesions, including multiple myeloma or fractures caused by trauma. The procedure is designed to acutely reduce and stabilise the fracture, restore vertebral body height, and correct the overall spinal deformity.
BKP can be performed under a local or general anaesthesia with the patient in a prone position and with the assistance of an imaging device known as "biplanar fluoroscopic imaging". The average procedure time takes less than one hour per treated fracture and generally requires a minimal hospital stay of less than 24 hours.
Stage 1: The deflated balloons are inserted into the vertebral body. BKP is performed from both sides of the bone (bilaterally) through two, half-inch or 1cm incisions, after which two orthopaedic balloons are placed inside the fractured vertebral body.
Stage 2: Both balloons are gently inflated within the collapsed area of the vertebral body, reducing the fracture and elevating the endplates.
Stage 3: Once maximum fracture reduction and deformity correction have been achieved, both balloons are deflated and removed. The fracture is then stabilized at its restored height by filling the cavity under low, manual pressure with high viscosity bone cement.
Post-operatively, most patients experience immediate and effective pain relief and therefore early remobilization. After the procedure, consultation is re-opened with the referring physician for a long-term follow-up in order to achieve optimal medical treatment for the underlying disease that was the probable cause of the fracture.
Results
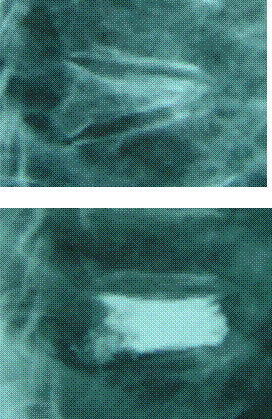
These images show the successful treatment of a three month old painful VCF in a 70 year old lady who sustained the fracture following a low energy mechanical fall.
BKP has been shown in both short and medium term follow-up, sustained benefits in the areas of spinal deformity correction, pain relief, early remobilisation, and quality of life.
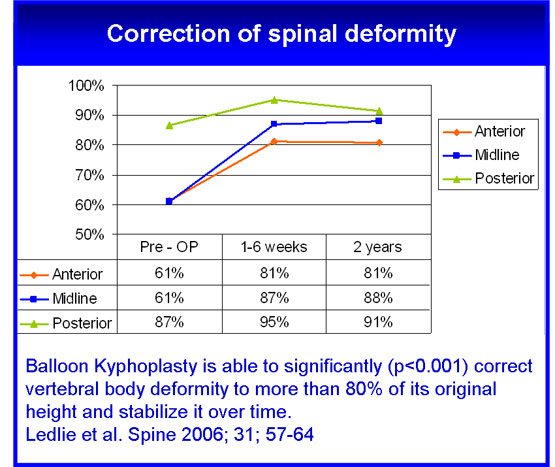
Spinal deformity correction
- On average, between 50 and 70% of lost vertebral body height is restored
- Excellent results have been seen in fractures treated within three months of onset of pain
Pain relief
- Most patients experience immediate pain relief as measured by visual pain analogue scale (VPAS) Scores, often within hours of the procedure
- Most patients depart from taking analgesic narcotic pain medication to none or simple over-the-counter oral analgesia
Early remobilisation
- Length of hospital stay can be as short as one to two days
- Some patients who were wheelchair-bound before their Balloon Kyphoplasty procedure walked out of the hospital upon discharge
Quality of life
- Patients report significant improvement in areas affecting quality of life, such as bodily pain, physical functioning, vitality, and mental health.
Summary
Balloon Kyphoplasty or BKP is an approved treatment option that combines efficacy and safety. Quality of life, mobility and daily functioning improve significantly following the procedure. For elderly patients with co-morbidities, polymedication and falling problems, consultation with a geriatrician and the primary care physician must me formally addressed. BKP is best performed in the context of a multidisciplinary team to guarantee optimal results.
Since 1998 more than 340,000 patients and more than 400,000 fractures have been treated with Balloon Kyphoplasty. The published cohort studies consistently show promising short and medium-term clinical and radiographic outcome results.
The time of a woman’s life when her ovaries stop releasing an egg (ovum) on a monthly cycle, and her periods cease
Full medical glossary








