This article discusses recent advances for the treatment of bone metastases including techniques such as balloon kyphoplasty and RadioFrequency Ablation. This will be of help to patients suffering from secondary cancer and would like to know what their treatment options are.
Contents
- Introduction to bone metastases
- How are bone metastases normally managed?
- Have there been any advances in recent years?
- Image guided RadioFrequency Ablation (RFA)
- Cryoablation
- Vertebroplasty / Cementoplasty
- Balloon Kyphoplasty
- Am I suitable for image guided tumour ablation?
Introduction to bone metastases
Most patients with cancer develop metastatic tumour deposits in their bones at some stage. These are most often as the result of secondary spread from primary cancers in the breast, lung, and prostate, but less common cancers such as those arising in the kidney or thyroid frequently spread to bone.
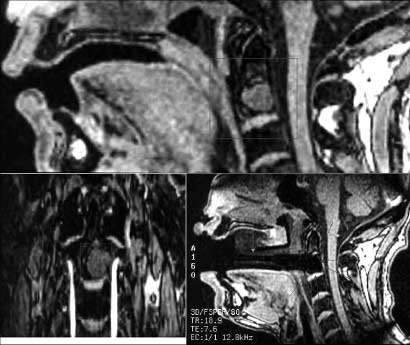
Bone metastases are most often found in the spine, pelvis, the upper femur and hip, humerus, and ribs. They cause pain and weaken the bones, increasing the risk of fractures, which can be very difficult to treat because of the destruction of normal tissue in the vicinity of the fracture, and the general health of patients at the time of the fracture which is often poor. In the spine, metastases can cause nerve damage and compression of the spinal cord leading to paralysis (Fig. 1).

Bone metastases are rarely treated surgically because it is rarely curative. It can also be difficult to get surgical access to the tumour without destroying too much healthy tissue, and adequate surgical excision can often excessively weaken the affected bone, increasing the risk of fracture.
How are bone metastases normally managed?
The options for managing bone metastases have traditionally been limited. In addition to adequate analgesia patients can be treated with chemotherapy and radiotherapy. Although these can be effective at limiting pain and growth in bone metastases they cannot always be used. In some patients the deposits do not respond to chemotherapy or radiotherapy, and other patients may not be able to have repeated treatments. Another disadvantage is that it can take several weeks for patients to get pain relief from bone metastases from these techniques.
Have there been any advances in recent years?
Over the past few years there have been considerable advances in techniques to target treatment only at the tumour in order to reduce the side effects and complications of chemotherapy, radiotherapy, and analgesia.
Although open surgery is playing a smaller role in the management of metastatic deposits there have been rapid advances in percutaneous techniques guided by various imaging technologies. Ultrasound is the imaging modality of choice for the real time visualisation of soft tissue structures but the sound waves cannot visualise bone or air filled structures very well. Computed tomography (CT) using x-rays is an excellent modality for imaging the body in cross section. It can show bone structure extremely well and can show fine detail within air filled structures such as lungs. CT shows cross sectional images and does not show bone anatomy in 3D real time. Where this is necessary fluoroscopy is used. This uses low doses of x-rays to continually screen the area of interest so the course of the probes being used can be followed in real time as they are guided into position. These imaging modalities are used either alone or together, depending on the targeted structure, to guide the percutaneous treatments.
There are a number of image guided percutaneous options to help to reduce the risk of fracture, stabilise the bone, and control pain. These are available in a number of specialist centres. They are:
- Radiofrequency ablation (RFA)
- Cryoablation
- Vertebroplasty / cementoplasty
- Balloon kyphoplasty
Image guided RadioFrequency Ablation (RFA)
In recent years image guided radiofrequency ablation (RFA) has become the treatment of choice for many patients with small numbers of liver or lung metastases, and as an alternative to surgery for the treatment of some patients with primary lung tumours.
RFA involves the insertion of a fine probe through the skin into the centre of the tumour. This is guided by the most appropriate imaging modality for the tumour being targeted. For liver this is generally ultrasound, with or without CT, while for lung it is generally CT (Fig. 2). Once in position high frequency radiofrequency energy is then passed through the probe, heating and destroying the surrounding tissue. This can be done in a very controlled manner to limit damage to healthy surrounding tissue. It can be done under a short and light general anaesthetic or under sedation, and often as a day stay procedure.
RFA tumour ablation has been shown to be both safe and effective and has been approved by NICE.
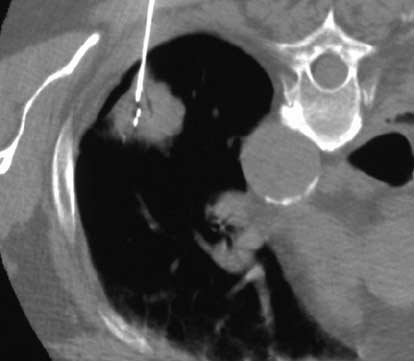
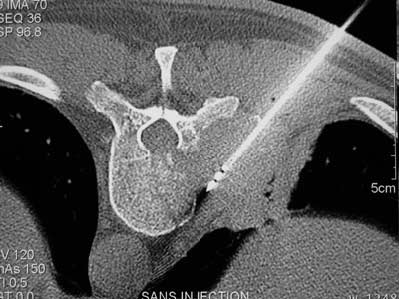
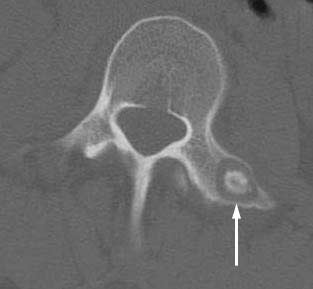
Image guided RFA has also been shown to be safe and effective for the management of patients with secondary bone tumours (Fig. 3). Guidance of the RFA probe into the tumour is performed using CT, and the metastatic deposit is usually heated to around 100°C for up to 15 minutes. If the tumour is large the probe can be re-directed so several RFA treatment cycles can be delivered during one procedure. Tumours can also be treated in very delicate areas such as in the spine. These cannot be treated using conventional techniques because of the risks of nerve root or spinal cord injury.
Image guided RFA is suitable not only for metastatic deposits. Osteoid osteomas are benign tumours of bone that tend to occur in young adults (Fig 4). They cause severe pain and conventional surgical treatment is destructive to surrounding tissue and bone. Image guided RFA has become the NICE approved treatment of choice for these rare tumours.
Cryoablation
In this technique freezing is used to destroy the tumour rather than heat. Probes that are a similar size to those used in RFA are inserted into the target tumour under CT guidance. Compressed argon gas is passed through the probes which is allowed to rapidly expand when it reaches the tip. This cools the tip of the probe to below freezing. An ice ball forms around the tip of the probe and spreads into the tumour, freezing and destroying the tumour cells. The process of tumour ablation can easily be followed as the ice ball is visible on CT. This technique has been used in extremely sensitive areas (Fig. 5).
Vertebroplasty / Cementoplasty
Vertebroplasty is the best known interventional procedure used to control pain from lytic vertebral body tumour deposits. It was first described in the mid 1980s to treat a painful haemangioma, which is a benign collection of blood vessels. It is most widely used to treat pain from osteoporotic vertebral body fractures, but it is also used to treat vertebral bodies affected metastatic tumours and by multiple myeloma, a malignant condition affecting bone marrow.
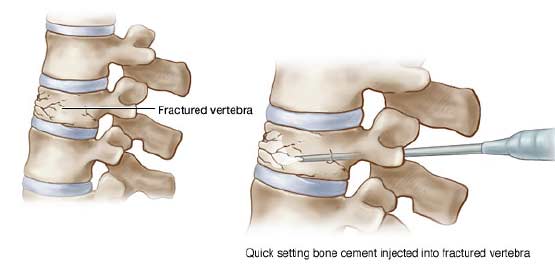
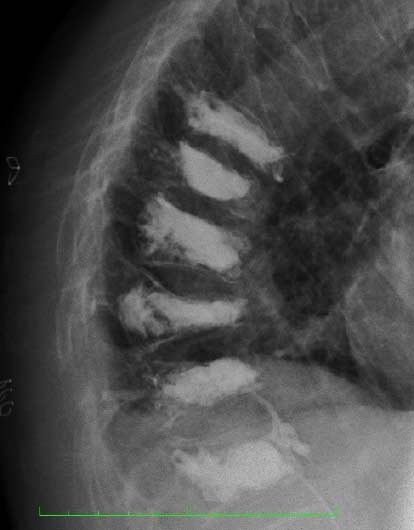
In vertebroplasty a large diameter needle is inserted into the vertebral body under continuous x-ray or CT guidance, through which polymethyl methacrylate (PMMA) bone cement is injected (Fig. 6). This heats up to around 60°C and hardens in a few minutes and they are able to walk and weight bear as soon as they wake from the short anaesthetic. Most patients who have undergone vertebroplasty experience a substantial reduction in their pain within 24 hours of the procedure, and many are able to stop strong painkillers altogether within a few days.
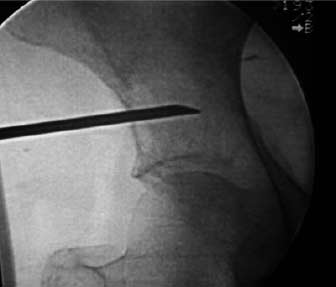
Cementoplasty is the injection of PMMA bone cement into lytic bone metastases (Fig. 7). It is similar to sacroplasty, a procedure where PMMA is injected into sacral insufficiency fractures, to stabilise them and to control pain. Cementoplasty is used either on its own or as an adjunct to radiofrequency ablation or to cryoablation of tumours.
Balloon Kyphoplasty
Balloon kyphoplasty is a recent development of the vertebroplasty procedure, which was borne out a desire to correct the forward angulation in the spine (kyphosis) caused by vertebral body fractures. This kyphosis is responsible for what we know as “Dowager’s hump” – the stooping posture and curvature of the spine often seen in elderly women.
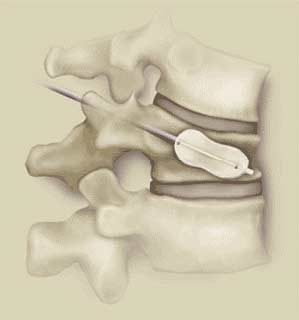
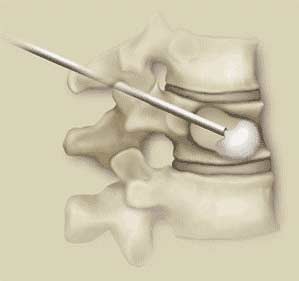
In BKP a balloon is first inserted into the fractured vertebral body (Fig. 8). It is then inflated to restore the vertebral body towards its pre-fracture height and shape. Kyphoplasty is mostly used for osteoporotic vertebral body fractures but it has been used for patients with metastatic vertebral body deposits although some specialists have expressed concerns about the possible risk of spreading malignant cells by the inflation of the balloon.
Balloon kyphoplasty is as effective as vertebroplasty at vertebral body stabilisation and management of pain. Its advantage is in its ability to restore some height and shape. Both techniques can be used in patients with multiple myeloma or osteoporotic vertebral body fractures (Fig. 9).
Am I suitable for image guided tumour ablation?
You may be suitable if you fulfil any of the following criteria:
- You have a benign osteoid osteoma – if this is the case RFA is the treatment of choice
- You have a small number of secondary bone tumours
- Your oncologist has said you cannot have more chemotherapy or radiotherapy
- Chemotherapy and radiotherapy have not been able to control your bone pain