This article discusses the causes and symptoms of heel pain and will be of help to anyone suffering from plantar fasciitis who would like to know what their treatment options are, whether surgical or otherwise.
Contents
- Anatomy
- Symptoms
- Who is at risk?
- What causes plantar fasciitis?
- Diagnosis
- Heel spurs
- Non-operative treatment
- Surgery to relieve plantar fasciitis
- Summary
Plantar fasciitis is a common cause of heel pain. It is often also known by the colloquial name of Policeman’s heel. Fortunately it is a self-limiting condition and in most patients (80-90%) the symptoms will get better within ten months.
Anatomy
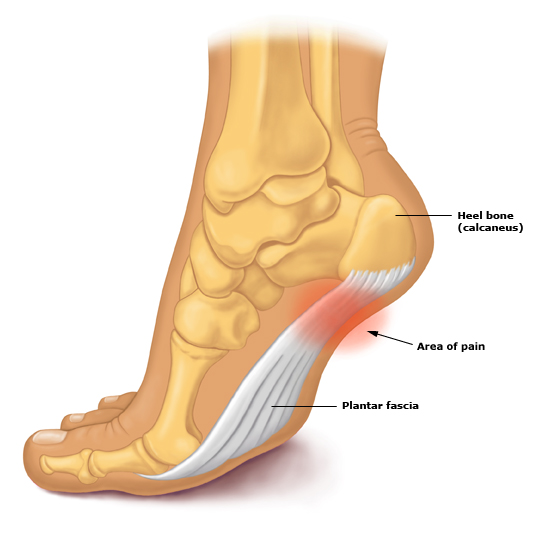
The plantar fascia is a strong fibrous band of tissue in the bottom of the foot which helps support its shape. It arises from the heel bone (calcaneus) and inserts into the toes. The heel bone is protected by a specialised pad of fat that cushions it when we stand. This also protects the attachment of the plantar fascia.
Symptoms
With plantar fasciitis start-up pain is common. This is a sharp or stabbing sensation in the region of the heel typically when getting out of bed in the morning or from getting up from a chair after a period of rest. Start-up pain often resolves but may be replaced by a dull constant aching or throbbing pain at the end of the day.
Who is at risk?
Patients who are overweight or who spend the majority of their day standing are at increased risk. Advanced age and a tight Achilles tendon as well as outside factors such as poor shoes also increase the risk. Recreational jogging does not increase the risk of plantar fasciitis.
What causes plantar fasciitis?
There are several theories as to the cause of plantar fasciitis but the most likely is that mechanical overload and excessive strain results in micro-tears in the tissue of the heel that in turn give rise to an inflammatory response. Repeated overload may hinder or prevent normal healing and this may result in chronic inflammation and degeneration of the tissues. This causes pain when the area is compressed.
Diagnosis
In the majority of cases your doctor will be able make the diagnosis from the symptoms and medical examination findings alone. Occasionally it is necessary to perform investigations to confirm the diagnosis or exclude other causes of the pain. Sometimes X-rays are used to rule out breaks (fractures) in the bone or very rare causes such as infection and tumours. Bone scans can also be used to exclude stress fractures. Ultrasound may be used to confirm the diagnosis, as it is very sensitive at measuring the thickness of the plantar fascia. Thickening of the plantar fascia is a firm sign of the condition. MRI scans are very sensitive at diagnosing a large number of conditions and also confirming the diagnosis of plantar fasciitis.
For direct access referral for plantar facitis treatment.
Heel spurs
Plain X-rays often pick up spurs of bone that are close to the attachment of the plantar fascia on the heel bone. These are very common and are not related to plantar fasciitis.
Non-operative treatment
There are a number of possible non-operative treatments and these are:
1. Self-treatment
Rolling your foot on a plastic bottle of hot or cold water is often very effective at reducing acute symptoms. It is best to experiment with hot and cold to find which you find most effective.
2. Stretching
Stretching of the plantar fascia and Achilles tendon, often supervised by a Physiotherapist, is very effective at relieving acute pain. There is some evidence that it may reduce the length of symptoms.
3. Orthoses
Soft rubbery orthoses, also known as heel-cups, are also effective at reducing the acute symptoms of plantar fasciitis when walking. There is also some evidence that they may reduce the duration of the condition.
4. Nocturnal dorsiflexion splints
A nocturnal dorsiflexion splint is a brace worn overnight holding the ankle at 90° and forcing the toes towards the shinbone. There is good evidence that these reduce start-up pain first thing in the morning and reduce the length of duration of symptoms. They can however be uncomfortable to wear.
5. Anti-inflammatory medication
Anti-inflammatory medication can either be taken in tablet form, an example being Ibuprofen, or in the form of a steroid injection. Oral anti-inflammatories can be very effective particularly early on in the disease. However, it appears that their effect is often limited to the first month only. Injections of steroids such as cortisone and local anaesthetic also have a significant effect in reducing pain in the short-term but do not appear to reduce the length of symptoms.
6. Extracorporeal shockwave therapy (Lithotripsy)
Extracorporeal Shock Wave Therapy involves passing shock waves from a probe through the tender area. This has a short-term effect of reducing pain and may reduce the duration of symptoms. Currently there are several studies being performed to measure its effectiveness in the long term.
Surgery to relieve plantar fasciitis
In addition to the non-operative treatments listed above, surgery can also be used to alleviate heel pain. Surgery to release the plantar fascia can be performed by either open or minimally invasive surgical techniques. Some surgeons also release the nerves in the region at the same time. This is reserved for patients that have severe limiting symptoms that are persisting beyond six months. This is effective in approximately 50% of patients but does have some associated risks. These include failure to relieve pain, infection, nerve injury resulting in numbness of the foot or a tender wound, bleeding, flattening of the foot, stiffness, wound tenderness, deep vein thrombosis (DVT) and pulmonary embolism (PE). Complex regional pain syndrome is a rare condition of pain and swelling that can occur post operatively and is poorly understood. It is treated with physiotherapy and pain medication. It may lead to chronic disability and pain if severe.
To ask a specialist about surgical options.
Summary
Plantar fasciitis is one of the most common orthopaedic conditions affecting the foot. In the vast majority of cases conservative, non-surgical treatment will be successful over a period of time although surgery may become necessary if the condition does not improve. A number of interesting studies are currently taking place into the effectiveness of shockwave therapy as a treatment for plantar fasciitis.
See also 7 Ways to Treat Plantar Fasciitis without need for Surgery by Consultant Rheumatologist, Dr Stephanie Kaye- Barrett.







