This article describes the treatments options available for a painful flat foot. Non-surgical treatment forms the mainstay in the first instance, with surgery reserved for resistant cases.
Contents
- What are the causes of a flat foot?
- What symptoms might I experience?
- What should I do if I have a painful flat foot?
- What are my options?
- What does surgery entail?
- What are the complications?
- Will I have a normal arch?
- I have heard about ‘titanium stents’ and minimally invasive surgery – is this an option for me?
What are the causes of a flat foot?
All children under three years of age have a flat foot which is entirely normal. The arch of the foot then develops through to adolescence, although many people continue to have a flat foot into adulthood. In the majority of cases, the problem is related to loose ligaments and joints, and tends to run in families. Up to 30% of the population have a flat foot, and in most cases it does not cause a problem.
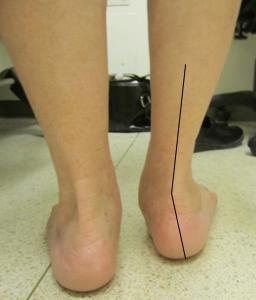
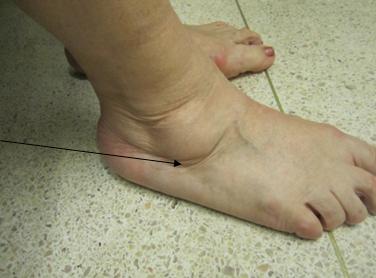
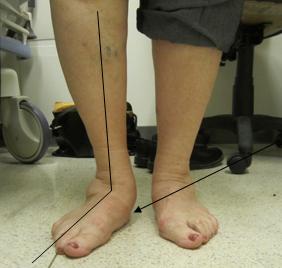
The most common cause of a painful flat foot is damage to the tibialis posterior tendon. This important structure runs on the inside of the ankle and is the principal stabiliser of the arch. This problem is also known as Adult Acquired Flat Foot deformity and usually occurs in middle-aged females, most of whom have had a slightly flat foot all their lives. The tendon stretches out over time and becomes less able to carry out its important functions. Occasionally an injury results in the tendon rupturing. Fig 1 (a,b and c) shows a typical flat foot.
Another common cause is an accessory (extra) navicular bone. You may be able to feel this bone, as it is usually prominent on the inside of your foot. The tendon, rather than attaching to the main body of the navicular bone, inserts onto this extra bone so its pull is less effective and the arch of the foot collapses. The main symptom is pain from the repetitive stresses placed upon this extra bone.
Rarely, a congenital problem results in two bones in the back of the foot being joined together. This is called a tarsal coalition. It results in a painful and stiff flat foot in children and tends to present between the ages of 8-15 years. You should seek the help of a Children’s Orthopaedic Surgeon, if your child has a stiff and painful flat foot.
What symptoms might I experience?
Pain is the most common problem. It is usually located on the inside of your ankle, where the posterior tibial tendon lies, and many times the problem is wrongly attributed to your ankle joint. Symptoms are typically worse first thing in the morning and after walking long distances. You may experience cramping or fatigue in your calf muscle, which tries to compensate for your weak posterior tibial tendon. In some patients the flat foot results in pinching of the tissues on the outside of your ankle (shown in Fig 1b), with swelling and pain. The abnormal structure of your foot can cause pressure areas and hard skin to develop, typically under your big toe, or on the inside of your heel.
What should I do if I have a painful flat foot?
You should ask your GP to refer you to a Consultant Orthopaedic Foot and Ankle surgeon, who is best placed to make a formal assessment. The diagnosis can often be made by asking you specific questions about your problem.
A full examination of your entire lower limb is required, as not infrequently a problem with your hip or knee alignment can cause a flat foot. A tight calf muscle can aggravate the problem and will be specifically examined. You will be asked to walk and to stand up on tip toes. If you are unable to tip toe on your affected side, this is a sign that your tendon is not working. Your ankle and foot joints will be assessed for flexibility.
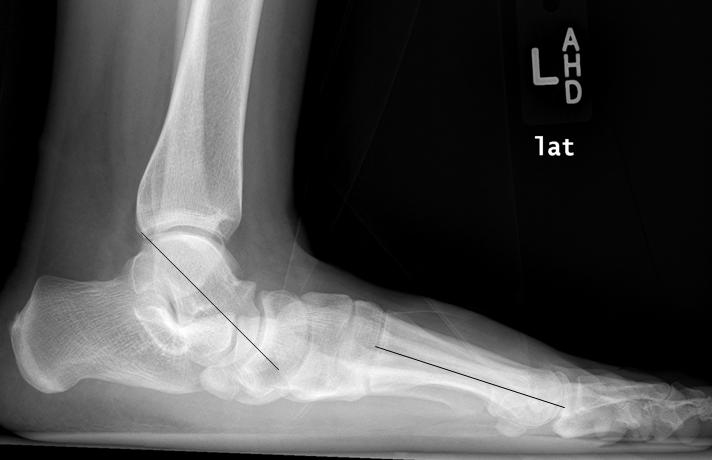
Weight-bearing x-rays will be organised to look specifically at your foot and ankle alignment and whether you have any ‘wear and tear’ or arthritis (Fig 2; click on the image to enlarge). An accessory navicular bone, if present, can also be detected. An MRI scan is often ordered to assess the tibialis posterior tendon, and is used to confirm rather than make the diagnosis.
What are my options?
The initial treatment does not involve surgery. You will be referred to the physiotherapy department, to undergo a formal calf stretching program. Your foot joints will be manipulated and gait training will also be undertaken.
You will be referred to an Orthotist, who will examine you and if indicated he/she will make an impression of your foot with foam or plaster and a custom-made insole will be manufactured. If you have a flexible foot, the insole will be built up on the inner aspect both along the arch and under the heel. This will help tilt your foot back into a more normal position and also provide support. If you have a stiff foot the insole will simply support the foot in its current position.
In some cases, the pain can be quite severe, and this usually indicates that the tendon is acutely inflamed. A period of rest in an Aircast boot often resolves this problem in the short-term.
These simple measures should be tried for three–six months before consideration of surgical intervention.
What does surgery entail?
You should discuss your options with a Consultant Orthopaedic Foot and Ankle Surgeon.
The surgery will depend on the following factors:
- The exact cause of your flat foot. (Below I describe the options for an accessory navicular bone and for tibialis posterior tendon dysfunction.)
- Whether you have a fixed or flexible deformity.
- Whether you have any arthritis.
Accessory navicular bone
Your tibialis posterior tendon will have been assessed with an MRI scan. In most cases the tendon with this problem is normal. Surgery involves removal of the extra bone and reattachment of the tendon. The shape of your foot will not change but your pain should be improved. In some cases the extra bone can be fused with your main navicular bone using screws. The advantage here is that the tendon does not need reattaching. You can discuss these options with your surgeon.
Dysfunctional tibialis posterior tendon
If you have a flexible foot, with no wear and tear, we try to perform an operation that preserves movement. Typically this involves cutting the heel bone and shifting it inwards. Screws are used to hold the heel in its new position. The diseased tibialis posterior tendon is removed as it is usually thickened and scarred. We then transfer the tendon that moves your little toes into the navicular bone, which then acts as your new tibialis posterior tendon and supports your arch. Additional procedures are added as necessary to put your foot flat to the ground and will vary from person to person. The most common of these will be a release of the calf muscle which is often found to be tight. A plaster cast is applied and no weight-bearing is allowed for six weeks. Thereafter an aircast boot is used to allow gradual weight-bearing, and physiotherapy started. The overall recovery period following this major surgery is six to nine months.
If you have arthritis or a stiff foot, a fusion will be performed. The joints at the back of your foot are repositioned to allow your arch to be restored, and are permanently fused (joined) together. Screws and plates are used to hold the bones stable during the healing phase. Following surgery the same protocol is used for rehabilitation.
What are the complications?
You could develop an infection or wound healing problems, although these often settle with simple wound care management and antibiotic prescription. You can develop a patch of numbness around the wound or beyond, although this rarely causes a significant problem.
Both the heel shift and fusion procedures occasionally fail to heal. This is called a non-union. If this occurs, another operation may be required to stimulate healing. With any major lower limb surgery, there is a risk of Deep Vein Thrombosis (DVT). Preventative measures will be employed both during and after surgery, and if you are considered high risk, you may require blood thinning injections for six weeks. Having said that, only a small percentage of patients I operate on are considered to be high risk.
Finally, if we have performed the heel shift and tendon transfer, this preserves movement, and whilst very successful in the medium term (five–ten years), the reconstruction can stretch out, and the flat foot can reoccur. If it does – a fusion procedure will be required.
Will I have a normal arch?
In most cases there will be an improvement in the arch, and it will be better supported. However, returning to a normal arch is rarely possible, and the principal reason for undergoing surgery is pain relief.
I have heard about ‘titanium stents’ and minimally invasive surgery – is this an option for me?
Minimally invasive titanium stent surgery otherwise known as ‘arthroereisis’, describes a small screw that is inserted into the space between the talus and heel bone. The idea is that it jacks open the joint, corrects the heel tilt and restores your arch. The National Institute for Clinical Excellence (NICE) guidance states that there is very weak evidence for its use in flat foot deformity, and if used, this should be within the context of a clinical trial, where outcomes and complications can be monitored closely. The implant is commonly used by non-medically qualified practitioners such as surgical podiatrists.
It is telling that Consultant Orthopaedic Foot and Ankle surgeons rarely use this device, and consider its use experimental. Personally, I am uncomfortable with this technology and I prefer to use methods that are tried and tested. Of most concern is that it has been suggested for use in children, without the support of the British Society for Children’s Orthopaedics, and with clear evidence that flat feet are considered a normal variant in a child. At the February 2012 American Orthopaedic Foot and Ankle Society meeting in San Francisco, its use was not even discussed by four world-renowned leading experts on flat foot deformity. You should seek the help of a Consultant Orthopaedic Foot and Ankle surgeon if you would like advice about your flat foot problem, or if you have been offered this device by another practitioner.







