Cosmetic foot surgeon
Mr Haroon Mann is Consultant Trauma and Orthopaedic Surgeon and expert in foot and ankle reconstruction. Mr Ash Mosahebi is a Plastics & Reconstruction Surgeon. We have therefore combined our skills with both orthopaedics and plastic surgery to bring the first integrated orthopaedic and plastics reconstructive and aesthetic foot and ankle clinic in the UK.
What is cosmetic foot surgery?
The trend of having a foot-lift to shorten, lengthen, or straighten unsightly toes, may sound simply aesthetic. However, in reality in our practice this is rarely the case, as a bony prominence or clinical deformity will usually lead to painful feet, as it’s difficult to find closed shoes that don’t rub or cause callosities. When patients present with a request for cosmetic enhancement of their foot, the improvement in a clinical deformity will result in an aesthetic or cosmetic improvement in the appearance, function and comfort of their feet too.
If non-surgical or conservative treatments have failed to alleviate the condition, or if the problem is advanced, then surgery may be the best option to remove, realign or enhance. This is where procedures are better described as reconstructive orthopaedic foot and ankle surgery, performed to lessen pain, improve the function and quality of life, as well as make your feet look great. Minimally invasive surgery has advanced our techniques and ability to improve the rate of recovery, with minimal scarring to maximum effect. We can use the latest laser treatment for unsightly nails and fungal infections.

Who needs reconstructive or cosmetic foot surgery?
Suffering painful feet or ankles is not something we should, or need put up with. Of course, the best form of prevention is to have a foot care routine to look after your feet and notice any problems forming. Painful corns and callosities can sometimes be a simple issue to deal with and skin blemishes and scars can cause underlying tethering of structures.
For those who suffer from Bunions or Hallux Valgus deformity there is a real clinical issue. The biomechanics of the deformity are very complex and once the toes deviate, little will stop the biomechanics of progression. The secondary effects are numerous, not only to the adjacent toes but to the ankle knee and spine. The abnormal distribution of weight and forces through the foot, transmit the forces to the ankle, knee and spine. Many patients report to me that their running and loading of the foot have improved in addition to the appearance of the foot which is a huge secondary bonus.
Even when faced with persistent foot pain, some people are still reluctant to consult an Orthopaedic Foot & Ankle doctor, but this is what they should be doing, as an orthopaedic and plastics foot surgeon is best equipped to suggest what can be done about a problem and recommend many treatments.
Are high heels the source of foot deformity?
There are two key causes of foot deformity leading to pain. The first is hereditary, as bunions and arthritis tend to be, the second is the shoes you wear, especially high heels, can exacerbate the problem.
Your feet carry your entire body weight for up to 10,000 steps a day without
complaint, so it’s important to look after them.
How to look after your feet
- Feet are an often neglected area of our bodies but are critical to our overall health, posture, balance and mobility.
- In our 20s to 40s our feet take a pounding. This is when women are wearing high heels, and we tend to be doing high-impact exercise and going to the gym.
- From our 50s the skin on our feet loses elasticity and thins, so supplements and rubs to keep them supple are needed, while circulation problems like cramp and plantar fasciitis (heel pain) become more common. Sometimes the underlying wear and tear needs to be addressed through surgery for conditions like arthritis, bunions and hammer toes.
- As well as physical pain and discomfort, there can be psychological damage if you feel you have to hide away deformed feet. I believe women should have the freedom to wear the shoes that they want to wear. Whether you'd rather wear heels or flats, I think it’s important to enable women to make that decision, and take pain out of the equation.
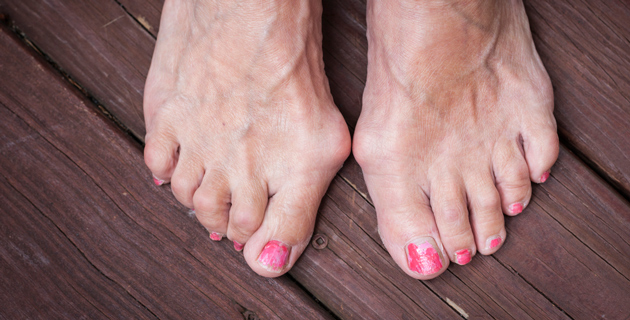
Common foot problems that can be helped by surgery
Bunions
Bunions are a deformity of the big toe joint, where a painful bony growth juts out on the joint at the base of the big toe, which forces the big toe to turn in at an angle towards the other toes. These can be very painful, not only where they rub on shoes, but also from deep within the joint. Pressure from your big toe may force your second toe out of alignment, sometimes overlapping your third toe. An advanced bunion may make your foot look deformed. If your bunion gets too severe, it may be difficult to walk. Your pain may become chronic and arthritis can develop.
SURGERY: The operation to correct them is now quick, and can be carried out in a day under local or general anaesthetic. The procedure involves cutting the bone and fixing it in its new position. This leads to narrowing of the foot without bony promminences
Adolescent bunions
Adolescent bunions appear in young teenagers, especially girls aged between 10 and 15, are at risk of developing an adolescent bunion at the base of their big toe. Unlike adults with bunions, a young person can normally move the affected joint or is occasionally hypermobile. More comfortable shoes rather than surgery is recommended, except in chronic conditions. Surgery before they are fully mature skeletally can result in the bunion returning.
Hammer toes
Hammer toes, also known as claw toes, are where the middle joints in the toes start to curl downwards, so the toes are bent. After a while the toes can become set like this. The smaller toes are particularly susceptible in pointy shoes. Painful corns can form on top of the toes that are pushed up, or on the tip of a toe, while extra pressure is put on the ball of your foot, which can result in calluses. It’s best to avoid tight, narrow and pointy shoes and try low-heeled, roomy shoes, to take the pressure off your toes. And do toe exercises, like using your toes to pick things up off the floor, or to scrunch and release a towel.
SURGERY: If left untreated, the toes can become fixed as the muscles tighten and cannot stretch out. Surgery involves removing the first joint in the toe and stiffening it permanently, called a fusion. Tight tendons are released, which are usually the cause of the deformity. This is usually carried out as an outpatient, and a wire is often used to hold the toe straight for four to five weeks.
Ganglions
Ganglions are fluid filled cysts which can form around joints and tendons and are common around the foot and ankle. The cyst can range from the size of a pea to the size of a golf ball, and though harmless, they can take years to disappear on their own. Sometimes they become uncomfortable or painful and can reduce movement of the joint. They seem to occur when the synovial fluid that surrounds a joint or tendon leaks out and collects in a sac. The first line of treatment is to drain the fluid using a needle and syringe, called aspiration.
SURGERY: If the lump causes pain and rubs on shoes, it can be removed by being cut out using surgery. Keyhole surgery can sometimes be used. Ganglions seem to have less chance of returning after surgery.
All procedures are best carried out by an orthopaedic surgeon
Morton's Neuroma
A neuroma is a benign thickening of the nerve. or of the tissue that surrounds the digital nerve leading to the toes. It occurs as the nerve passes under the ligament connecting the toe bones (metatarsals) in the forefoot.
Morton's neuroma most frequently develops between the third and fourth toes, usually in response to irritation, trauma or excessive pressure. The incidence of Morton's neuroma is 8 to 10 times greater in women than in men.
Normally, there are no outward signs, such as a lump, because this is not really a tumour.
Burning pain in the ball of the foot that may radiate into the toes. The pain generally intensifies with activity or wearing shoes. Night pain is rare.
There may also be numbness in the toes, or an unpleasant feeling in the toes.
Runners may feel pain as they push off from the starting block. High-heeled shoes, which put the foot in a similar position to the push-off, can also aggravate the condition. Tight, narrow shoes also aggravate this condition by compressing the toe bones and pinching the nerve.
Diagnosis and Treatment
During the examination, your physician will feel for a palpable mass or a palpable "click" between the metatarsals. He or she will put pressure on the spaces between the toe bones to try to replicate the pain and look for calluses or evidence of stress fractures in the bones that might be the cause of the pain. Range of motion tests will rule out arthritis or joint inflammations. X-rays may be required to rule out a stress fracture or arthritis of the joints that join the toes to the foot.
Initial therapies for Morton's Neuroma are nonsurgical and relatively simple. They can involve one or more of the following treatments:
- Changes in footwear. Avoid high heels or tight shoes, and wear wider shoes with lower heels and a soft sole. This enables the bones to spread out and may reduce pressure on the nerve, giving it time to heal.
- Orthoses. Custom shoe inserts and pads also help relieve irritation by lifting and separating the bones, reducing the pressure on the nerve.
- Injection. One ultrasound guided injection of a corticosteroid medication can reduce the swelling and inflammation of the nerve, bringing some relief.
Several studies have shown that a combination of roomier, more comfortable shoes, nonsteroidal anti-inflammatory medication, custom foot orthoses and one injection provide relief in over 80 percent of people with Morton's Neuroma. If conservative treatment does not relieve your symptoms, your Orthopaedic surgeon may discuss surgical treatment options with you. Surgery can resect a small portion of the nerve or release the tissue around the nerve, and generally involves a short recovery period.







