This article discusses bunions and outlines the various treatment options and recovery process for this common foot condition.
Contents - bunions
- What are bunions?
- What simple non-surgical methods can we use to treat bunions?
- When would surgery be appropriate for bunions?
- What does surgery for bunions entail?
- Is surgery for bunions painful?
- The recovery process following surgery for bunions
- Conclusion
What are bunions?

Bunions (the medical term is Hallux Valgus) are just an overgrowth of new bone and soft tissue. This well-known deformity at the base of the big toe is more than just a bump or bunion on the outer side of the foot (click on image to enlarge). The actual prominence of this bump arises from the head of the metatarsal bone of the big toe drifting inwards towards the smaller toes. When the foot is squeezed into a shoe there is then an increased outward directed pressure on the big toe that compounds the problem. Initially, the toe corrects itself when the shoe is removed but with time the deformity becomes stuck down and fixed. In addition, the other bones of the big toe push the metatarsal head more into the middle, worsening the deformity. However, only half the cases of bunions are related to poor footwear, as many patients also have a positive family history for bunions.
What simple non-surgical methods can we use to treat bunions?
Appropriate shoe wear is really the key treating bunions without surgery. I always advise patients to wear soft lace-up leather shoes or trainers for commuting to work. A shoe with a strap or laces means that you are less dependent on curling your toes (the site of the pain!) to keep the shoe on. Keep a pair of formal shoes under your desk for meetings. Heels greater than one inch are best avoided as the foot tends to slide down the shoe squashing the toes into the toe box of the shoe. Silicone spacers or bunion cushions may help but can widen the foot further, making shoe wear more difficult.
When would surgery be appropriate for bunions?
If you have tried the above measures but your foot still hurts on a fairly regular basis or if you start to develop problems with the second toe then surgery may be appropriate.
What does surgery for bunions entail?
By the time most people suffering from bunions consult to their GP the deformity is usually advanced which means that the metatarsal needs to be broken and reset so that the foot is narrower and of a more natural shape.
For a moderate deformity, the bone is broken (osteotomy) close to the metatarsal head, using a chevron shaped bone cut. I usually do this procedure through a very small incision, no longer than the bunion itself (minimally invasive). The deforming tendon is cut through a stab incision under x-ray guidance. The bone is cut with a small saw and the end of the bone moved outwards. As the bone has been broken I fix it with a small screw (click on images to see before and after images of surgery). As it does not have a head it cannot be felt and is usually left in place forever.
More advanced deformities need correction closer to the apex of the deformity at the base of the metatarsal. The osteotomy I use for this is the scarf osteotomy, which is powerful, popular and proven. Here the metatarsal has to be split along its length with a specialist bone cut so the incision will be longer. The scar fades with time but as it is on the side of the foot it is readily visible when standing or in ballet pumps. If the joint is very arthritic then a fusion procedure may be necessary.
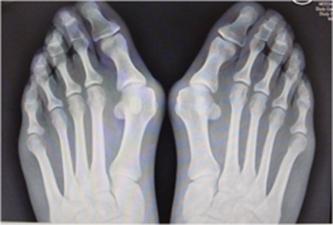
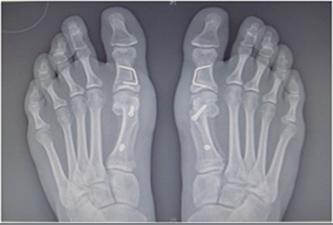
In severe deformities or in cases where surgery has previously been done, the other toes may also start to develop problems. Common patterns include pain under the lesser metatarsal heads, dislocation of the toes and formation of hammer toes. This is technically more difficult to treat and this is often because the bunion has been left too long. Nevertheless good results can still be obtained if we break and fix the other toes as required so as to leave a forefoot, which is more level and comfortable. The lesser metatarsals may be broken and fixed with a small screw (Weil osteotomy) and the hammer toes corrected.
Is surgery for bunions painful?
Surgery for bunions is not painful and this is one medical area where we have made dramatic progress. The main reason for why bunion surgery was painful in the past was that bones were held with plaster or pins only, allowing grating from the cut bone ends and a chance that the fixation could be lost. We now use small screws and specialist bone cuts to ensure a solid fixation of the bone. This allows earlier weight bearing and movement in the toes, ensuring faster rehabilitation and a better long-term outcome. In surgery, the use of selective ankle nerve blocks with a long acting local anaesthetic numbs the toes, minimising initial post-operative pain.
The recovery process following surgery for bunions
Surgery for bunions is most commonly performed for patient comfort under a general anaesthetic although it is also possible to have the procedure under local or spinal anaesthetic.
An ankle block will be administered in the operating theatre. This numbs the small sensory nerves around the foot helping to control the pain and to minimise the dose of general anaesthetic. Your foot will be heavily bandaged to protect it and to reduce the swelling. The gauze bandage that is applied in theatre in a sterile environment will stay on for two weeks and there will be no plaster cast.
The physiotherapist will issue you crutches and a special surgical sandal to wear. The crutches are not essential but as the foot is sore when weight bearing you may prefer it. It is important that the bandages are kept clean and dry. You can shower using a special bag (like a shower-cap) that keeps the bandage dry.
You will be given medicines to take home to control the pain. The nurse will go through the medicines with you, including how often and when to take them. There will be a combination of strong and weak pain killers.
When you feel comfortable and ready you will be allowed to go home. You should have made arrangements to be picked up from the hospital and have at least someone staying with you overnight if you are being operated on as a day-case.
As a day-case patient, you normally go home about 3–5 hours after the surgery. If you are staying in hospital overnight, you will be discharged around 10am the next day.
The next day: The block will start to wear off so you will start to feel sorer. You can pre-empt this by taking the painkillers. You can get up to use toilet but it is best to try to rest for the next few days.

Day 3 – 7: You should try to rest with your leg elevated for as much of the time as you can. Whenever the foot is put down, it will swell and become sore. It is normal to see mild bruising and some dry blood on the foot. By the end of this period the post- operative pain should have significantly reduced.
Day 7 – 14: Things get a bit easier. Do still elevate the foot as much as possible. You can start working from home but you must try and keep the foot up. Those patients that elevate their foot report minimal post-operative pain. You may walk short distances within the home or to a car during this period, using the surgical sandal.
Day 12 – 16: You will have an appointment at the dressing clinic when you will usually see the team nurse and then your surgeon. At this appointment, the bulky dressings are removed. If necessary, the tails of the stitches are trimmed back and Steristrips, which are paper dressing’s, may be applied. With larger corrections, a toe alignment splint will be applied, which you need to try and wear for at least 16 hours a day. Simple toe bending exercises will be demonstrated to you. You will leave with the same surgical shoe on.
After bunion surgery, the big toe joint becomes very stiff. This can be prevented by regularly performing a range of motion and stretching foot exercises. Until this appointment, no exercises are required as only rest and elevation are to be observed by the patient. These exercise routines will help you to recovery quickly after bunion surgery, prevent stiffening of the big toe joint and prevent painful scarring. You can start driving if the surgery was on your left foot and you have an automatic car but as motor insurance companies vary in their policies it is advisable to check with them first. You can now also shower the wound.
Day 21: You can consider flying at this stage; although with long-haul flights you should expect some swelling and pain in the foot. If your home is abroad then you can fly with special precautions much earlier in the post-operative period.
Skin emollients such as Aloe Vera, Vitamin E or Bio-oil may be applied around the healing wound. Once the wound is totally closed, these lotions may be applied over the wound. Swimming can be started if the wound is dry.
Day 28: It is now possible to start full weight bearing in a more regular shoe. The bone has not fully mended but is ‘sticky enough’ to ensure that walking short distances should not be a problem. At this stage, the foot is still too swollen to fit into your normal shoes. If you don’t have a pair of loose shoes then plan ahead and pick up a cheap pair of wider, loose shoes (with a strap over the ankle or a lace). Trainers are a good option or your existing running shoes with the far end laces left loose or removed is a supportive shoe. A rubber ‘croc’ type shoe possibly a size up is also a good option. It may be 8–10 weeks or longer before you can wear your broader old shoes.
Week 5 – 6: At this stage you will have a follow-up appointment with your surgeon. You will find your mobility will improve over the next few weeks however there is no real merit in walking long distances.
When you return to work, travelling outside of the rush hour is a good way of phasing back into work although the first few days are always slightly miserable as you are not able to keep the foot up as easily in the office. Low impact gym work such as the exercise bike or cross trainer can be started. Driving is fine but again check with your insurance company. If you require physiotherapy then your surgeon will refer you for it at this stage.
Week 12 Onwards: Now you can start enjoying the foot but the final shape of the foot in terms of the swelling and fading of the scar can take 6–9 months. Running can be started at 10–12 weeks. Other high impact exercise can be started at the same time. A gentle heel can be introduced and you can move into higher heels with time (although within limits as we know that they are not great for your feet).
Conclusion
Considerable advances have been made in recent years in the technique for treating bunions with surgery and it has become less painful and the recovery period much quicker than previously.







