Contents: - What is Atrial Fibrillation
What is Atrial Fibrillation?
Atrial fibrillation is a rapid, irregular heart rhythm which can develop as the heart ages. Ageing causes the cells within the atria (the top 2 chambers of the heart) to conduct electricity increasingly abnormally. Much like our skin looks different in our 60s, 70s and 80s, the tissue of the heart ages too. Rather than smooth ripples of electricity conducting through tissue, electrical chaos develops in an irregular pattern. This causes the heart to become much less efficient and heart function is reduced.
Rapid, irregular palpitations, breathlessness, chest pain lightheadedness and tiredness
AF can cause rapid, irregular palpitations, breathlessness, chest pain, lightheadedness and tiredness. However, it causes no symptoms at all in about a quarter of patients, and yet their risk of stroke is the same as if symptoms are present. The risk of developing AF increases with increasing age and it is also very frequently seen in patients with high blood pressure or other cardiac problems like heart attacks, valve disease or other heart muscle problems. However, AF can also occur in people with no other medical problems.
AF - The Most Common Heart Rhythm Disorder
Atrial fibrillation is the most common heart rhythm disorder in the developed world and it is estimated that more than one million people in the UK have this condition. Atrial fibrillation, or AF for short, is the 2nd most common cause of stroke in the UK and the most common in the non-elderly population. Overall, it increases the risk of having a stroke by a factor of 5 and can also lead to heart failure in some patients.
Atrial Fibrillation (AF) and risk of stroke
When the electrical activity in the atria becomes chaotic, blood can stagnate inside them and this can cause a clot to form inside the heart, particularly in what is called the left atrial appendage. This is a tube-like chamber (a bit like the appendix in the bowel) attached to the left atrium. When clots form here they can dislodge, travel through the heart and circulation to the brain, where they result in a stroke.
To identify patients who are at risk of stroke when they have atrial fibrillation, we use a scoring system called the CHA2DS2-VASc scoring system.
CHA2DS2VASc score
H = Hypertension (or high blood pressure)
A2 = Age over75
D = Diabetes
S2 = Stroke or TIA (transient ischaemic attack, or ‘mini-stroke’)
V = Vascular disease (heart attack or other arterial disease)
A = Age over 65
Sc = Sex category (female = 1 point)
If you have or have ever had one of these conditions you score one point for each, except Age over 75 or Stroke/TIA, which each count as 2 points, hence CHA2DS2VASc score.
What your CHA2DS2VAScscore means
If you have a CHA2DS2VASC score of 1 or more, it is recommended you take warfarin (or one of the newer types of anticoagulant medications, the NOACs) for the rest of your life to reduce your risk of stroke. So, if you are 65 or older and are diagnosed with atrial fibrillation, it is recommended you are treated with an anticoagulant and not aspirin, which is now known to have no benefit.
The only exception to this rule is if your only CHADS-VASc point is due to female gender. We know women are at slightly higher risk of stroke than men if they have AF but this only becomes relevant if women are over 65 years old or if they already score another point on the CHADS-VASc scoring system. In other words, if you are a 64 year old woman and have no other medical problems, you still score 1 point but do not need an anticoagulant. However, once you turn 65, you will need an anticoagulant and you will score 2 points.
How can Atrial Fibrillation be Diagnosed and Identified?
If you develop any of the symptoms described above, a simple check of your pulse can confirm if it is beating irregularly. To diagnose AF, an electrocardiogram (ECG or heart tracing) is needed when you feel palpitations or other symptoms. If your symptoms are intermittent, you may need to wear a heart monitor for a longer period of time to try and capture an episode.
Atrial fibrillation can also be easily identified in patients with pacemakers or defibrillators when their device is checked.
Occasionally it is necessary to implant a small heart monitor under the skin to diagnose a patient’s palpitations, if they are very infrequent or if you have had a stroke which is thought could have been due to undiagnosed AF.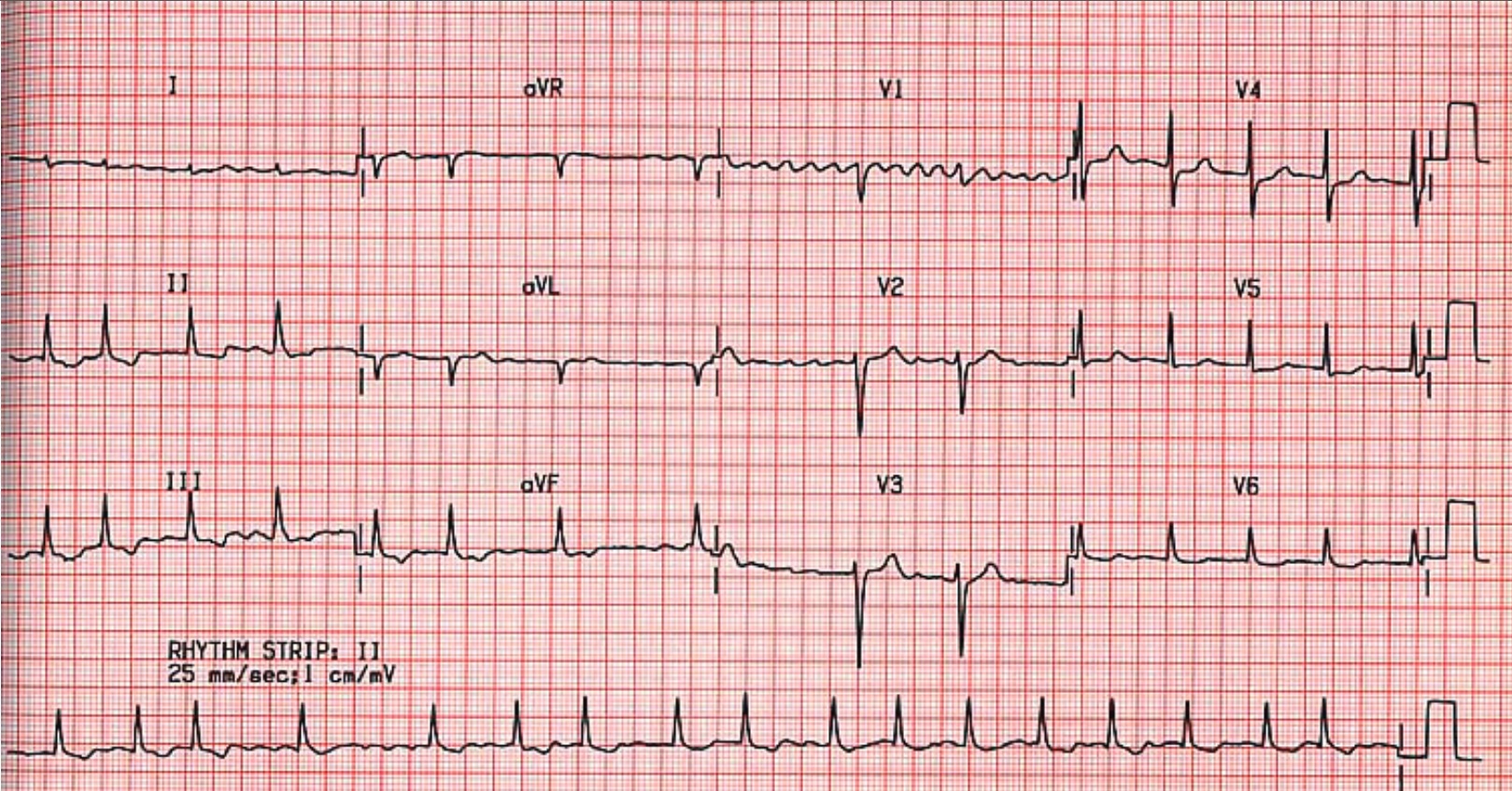
ECG of atrial fibrillation – irregular and rapid, chaotic atrial activity seen under lead V1 (the wiggly line!)
Jump to:
-
Treatments for Atrial Fibrillation
-
Complications from Catheter Ablation for Paroxysmal Atrial Fibrillation (PAF)
-
Atrial Fibrillation Ablation FAQs
About Dr Oliver Segal MD FRCP FHRS
- Qualified from King’s College Hospital in 1995
- Trained at St. Bartholomew’s, London Chest, St. Mary’s and St George’s Hospitals in London in cardiology and electrophysiology. Awarded a fellowship in pacing and electrophysiology at the world-renowned unit of electrophysiology in London, Ontario, Canada in 2007 with Prof. George Klein.
- Won first prize for Clinical research for his work on mapping ventricular tachycardia at the Heart Rhythm Society Young Investigator Award in San Francisco, USA in 2004.
- Appointed as full time Consultant Electrophysiologist at The Heart Hospital, University College London Hospitals in 2008. He is also Honorary Consultant at Homerton Hospital, Queen Elizabeth the Queen Mother Hospital, Margate and the Great Ormond Street Hospital.
- Has admitting rights at The Harley Street Clinic, Wellington Hospital, London Bridge Hospital, BUPA Cromwell Hospital and St. Anthony’s Hospital Cheam
- Has over 10 years experience in electrophysiology and devices, and has performed more than1500 ablation procedures and over 850 device implantation procedures
Dr Oliver Segal's Personal Philosophy
“Patients deserve the best quality healthcare provided by highly trained professionals. I am proud to be able to offer the state of the art in treatment for arrhythmiapatients at some of the UK’s leading private and NHS Hospitals.”







