This article, by an expert in Gynaecological Cancers, explains the treatment options for cervical cancer and will be of assistance to women who have been diagnosed with cervical cancer and would like to know what the next steps involve.
Vaccination for HPV is thoroughly recommended in most cases to prevent cervical cancer. For information on getting yourself vaccinated – click here.
Contents
- How is cervical cancer treated?
- Cervical cancer staging
- Very early cervical cancer
- Early cervical cancer
- Radical trachelectomy
- Radical hysterectomy
- Complications of surgery
- Large stage 1 or more advanced cancers
- Side effects of chemo radiation
- Widespread cancer (Stage IV)
- Other complications
How is cervical cancer treated?
Cervical cancer should be treated in a specialist unit known as a cancer centre. A team of experts, known as a multidisciplinary team, will be involved in your care. The doctors who look after this disease are gynaecological oncologists (surgeons) or clinical oncologists (radiotherapy experts). Other members of the team include a Clinical Nurse Specialist (CNS or MacMillan Nurse), and a psychologist who are available to support you and look after your social and psychological needs throughout treatment and beyond. Not all hospitals have this expertise available and you may have to be referred from your local hospital to a cancer centre.
Cervical cancer can be treated by surgery or by a combination of chemotherapy and radiotherapy, known as chemoradiation. The treatment you are offered will depend on the type of cancer, the extent of it and your personal circumstances. In order to plan treatment, the doctors will need to undertake a series of tests, known as staging tests. The stage of a cancer describes the extent of the cancer. Cancer spread is known as metastasis.
Cervical cancer staging
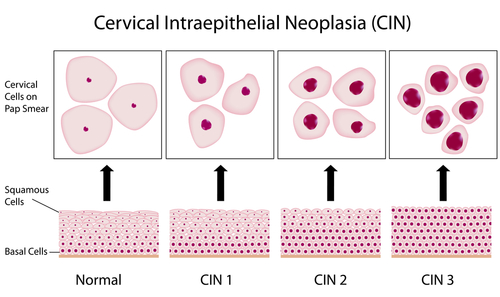
There are four stages of cervical cancer:
Stage II: Beyond cervix to side of cervix (parametrium) or upper vagina
Stage III: Into pelvis further into parametrium or lower vagina
Stage IV: Beyond pelvis to bladder, bowel or distant organs
One of the first tests performed is an examination under anaesthesia (EUA). This involves a short anaesthetic to enable the doctors to examine you thoroughly without causing you pain. The cervix is examined and further biopsies may be taken. A small telescope, known as a cystoscope, inserted through the urethra (waterpipe), is used to examine the bladder, which sits just in front of the cervix and may be involved in the cancer in more advanced stages. The lower bowel (sigmoid) may also be examined (sigmoidoscopy). This procedure allows the doctors to determine if the cancer is confined to the cervix or if it has spread beyond the cervix and it helps them to select the best treatment for you.
You may also be required to undergo a number of scans. An MRI (Magnetic Resonance Imaging) may be used to examine your pelvis. It gives detailed information about the anatomy and is better at detecting early spread than the EUA. In addition, you may be asked to have a CT (Computerised Tomography) scan of your chest and abdomen to look for enlarged lymph glands and other metastasis.
Once these tests are completed, your doctor can make a recommendation for treatment which he or she will discuss with you.
Very early cervical cancer
Very early cervical cancer is known as microscopic disease. Most of these cancers are screen-detected and can be treated by a cone biopsy. A cone biopsy is a small simple procedure during which the area on the cervix from which abnormal cells rise can be removed with a knife, under general anaesthesia. The biopsy is examined under a microscope in the laboratory and if all the abnormal cells are removed, no further treatment is necessary but you will be kept under review and seen regularly by the specialist for at least five years.
The advantage of a cone biopsy is that you can go on and have babies. Occasionally, the procedure can cause the cervix to be weak (Incompetent), putting you at risk of miscarriage or premature labour. It is important that when you are pregnant, you let your obstetrician know you have had a cone biopsy. He/she will monitor the cervix and if it shows signs of becoming weak, can put a stitch in to stop you from loosing the pregnancy.
Early cervical cancer
Cancers that are confined to the cervix but big enough to be seen by the naked eye can, in the majority of cases, be treated with an operation. The type of operation you are offered will depend on the size of the cancer and if you wish to have children.
Radical trachelectomy
This is a procedure designed for women who wish to maintain their fertility. For this procedure to be suitable, the cancer should be less than 2cm in diameter, with no other worrying features. A trachelectomy involves removing the cervix, the area surrounding the cervix (parametrium) and the upper 2cm of the vagina, in order to remove the tumour completely, with a zone of normal tissue around it. The procedure is done through the vagina so there are no cuts on your tummy. In addition, the lymph glands in the pelvis are removed using keyhole surgery (laparoscopic pelvic node dissection). All the specimens are sent to the laboratory for careful analysis. If the tumour is completely removed and the lymph nodes show no sign of cancer spread, no other treatment is required but you will be asked to remain under hospital care for at least five years.
This procedure is relatively new, having been introduced in France in the early 1900s. Despite this, experience has shown it to be a safe procedure. There is a higher risk of miscarriage and premature labour so a stitch is inserted into the bottom of the womb to prevent you from losing pregnancies. All future babies will have to be born by Caesarean section.
Radical hysterectomy
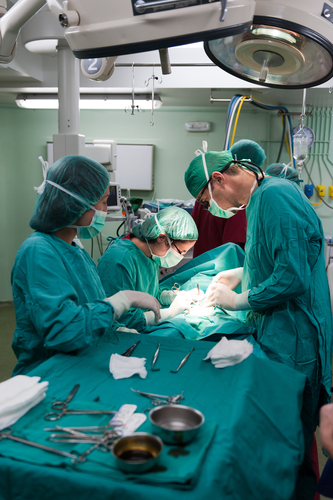
Radical hysterectomy has been used to treat cervical cancer for over 100 years. It involves removing the cervix, the upper vagina, the parametrium and the womb as well as the lymph glands in the pelvis. This operation can be done by keyhole surgery (laparoscopy) or through a bikini-line cut in your tummy.
All the organs removed are sent to the laboratory for analysis. If tests show that the cancer has been removed, with a safety zone of normal tissue around it and that the lymph glands show no sign of cancer spread, no further treatment is required. You will need to be kept under hospital care for at least five years.
If however, the cancer reaches the margins or the lymph glands have signs of cancer spread, then surgery alone is unlikely to cure the cancer and chemo radiation will be recommended. As a rule, doctors prefer to avoid giving chemo radiation after surgery as this doubles the risk of side-effects. Thus, you will only be offered surgery if the doctors are fairly certain that the cancer can be removed and that the lymph nodes are likely to be negative.
Although a radical hysterectomy is a complex procedure, in expert hands, the side effects and complications are few.
Complications of surgery
Any big operation can cause bleeding and, if it is necessary, you may be given a blood transfusion. In addition, the following specific risks are associated with this procedure.
- Loss of fertility potential. The womb is removed which means you cannot carry your own pregnancies. In young women, the ovaries can be left, allowing the potential for in vitro fertilisation (IVF) and pregnancy carried by a surrogate. Leaving the ovaries also prevents an early menopause. In women who have already undergone the menopause, removal of the ovaries is recommended as they no longer have a function.
- Damage to internal organs. There is a small risk of accidentally making a cut in the bladder, the ureter (tube that carries urine from kidney to bladder) the bowel or blood vessels. As long is this is recognised at the time of surgery, the cut area can be stitched up and there should be no long term problems. If the injury is not recognised, then a fistula can occur. A fistula is an abnormal connection from one organ to the next and can occur between the bladder and vagina, for example, leading to a loss of urine through the vagina. This will need further surgery to rectify. In expert hands, these complications occur in approximately 1 in 100 women having this type of surgery.
-
Nerve damage. Two nerves may be at risk during removal of the lymph glands. The genitofemoral nerve supplies the sensation to a small area of skin in the inner thigh. If this is cut or bruised, there may be a loss of sensation. Bruising will recover in time and recovery may be heralded by tingling or pins and needles in the area. If the nerve is cut, it cannot be repaired but most women are not too disturbed by it’s absence. The obturator nerve supplies a group of muscles on the outer thigh that help to bring the legs together. If this is cut it can lead to some difficulty walking but this can be improved by physiotherapy.
During the hysterectomy itself, some nerves, known as the parasympathetic nerves, may be disturbed. These nerves are responsible for emptying the bladder or bowel. Although rare, the bladder can become lazy after this procedure and not empty properly, leading to urinary retention. Doctors are aware of this complication and will check that you can empty your bladder properly by using a small scanner to check how much urine is left in your bladder after you have passed water. If this test shows that you are retaining urine, you will be taught to self-catheterise. This involves passing a thin plastic or metal tube through the urethra (water pipe) into the bladder to empty it. Over time, the bladder starts to work better and you can stop self catheterising. Similarly, the bowel may become lazy, making you more prone to constipation which can be managed by dietary modification and the judicious use of laxatives. - Lymphoedema. Lymph is a clear, colourless fluid that circulates throughout the body like blood. It carries immune cells and runs in little vessels called lymphatic channels. Lymph nodes are small glands which lie along the lymphatic channels and trap foreign bodies such as bacteria, viruses or cancer cells. Removing the lymph glands in the pelvis can sometimes cause the lymphatic fluid to accumulate in the legs, leading to swelling known as lymphoedema. Once this occurs, it cannot be cured, but can be kept under control by a combination of specialist massage and garments designed to compress the legs. Fortunately, it is an uncommon complication and occurs in less than 1 in 20 women undergoing this type of surgery.
Large stage I or more advanced cancers
These cancers are treated by chemo radiation. This involves giving radiotherapy to the pelvis with a weekly dose of a chemotherapy drug called cisplatin, given by drip. It is important to realise that cisplatin will not cause you to loose you hair.This treatment has similar cure rates to surgery and is chosen instead of surgery if the cancer is too big to be removed. Radiotherapy works by killing cells and cancer cells are more likely to be affected than normal cells because they grow at a faster rate. However, other cells can be affected and this leads to side effects.
Side effects of chemo radiation
- Premature menopause: It takes only a small dose of radiotherapy for the ovaries to stop working. Therefore young women will undergo an immediate menopause. To prevent this from happening, your surgeon might offer a procedure called ovarian transposition before you start your radiotherapy. This involves moving the ovaries, using key hole surgery, from the pelvis to high up inside the abdomen where they are safe from the effects of radiotherapy.
- Loss of fertility potential: The womb will not work after radiotherapy so you will not be able to carry a pregnancy. If you have a partner you may be able to undergo a cycle of IVF and have the embryos stored, provided this does not delay your treatment. It is then possible for a surrogate mother to carry these embryos and you will have your own biological baby. The doctors will discuss your suitability for this option with you.
- Damage to lining cells: The cells that line all the organs in the pelvis are also relatively fast-growing and are thus susceptible to the effects of radiotherapy.
- Vaginal lining: This can become thin and scarred, causing the vagina to narrow. You will be instructed to use dilators or have regular sex to prevent this complication.
- Bladder lining: Damage to the lining of the bladder can cause cystitis-like side effects with burning when passing water, frequency and occasionally blood in the urine. These symptoms can be treated with tablets and bladder training by specialists known as uro-gynaecologists.
- Bowel: The bowel is very susceptible to the effects of radiotherapy. Side-effects to the large bowel can cause diarrhoea, involuntary loss of stool and bleeding from the back-passage. Damage to the small bowel can cause diarrhoea and poor absorption of nutrients. Rarely, fistulae and strictures can affect the bowel. Specialists known as gastroenterologists can help manage these side effects.
Widespread cancer (Stage IV)
If cancer has spread to other organs, it is unlikely to be curable. In these circumstances, the doctors will focus on improving your quality of life by providing treatment to alleviate your symptoms. This is known as palliative care and the treatment offered will depend on the symptoms you are experiencing. For example, a small dose of radiotherapy may be required to stop excessive bleeding. The doctors will always explain the treatment offered and what it can be expected to achieve.
Other complications
A diagnosis of cancer and its treatment can have profound psychological side effects and women can become fearful and anxious. It is important to acknowledge these feelings and accept help and support from the CNS and psychologist.
For further information on the author of this article, Consultant Gynaecologist, Dr Adeola Olaitan, please click here.
The time of a woman’s life when her ovaries stop releasing an egg (ovum) on a monthly cycle, and her periods cease
Full medical glossary




