If you suffer from irritable bowel syndrome, you’ll already know that this debilitating illness can be difficult to treat. Top London nutritionist Stephanie Moore explain how a holistic approach can help heal your gut, and free you from the everyday misery of IBS.

What is irritable bowel syndrome?
IBS is a combination of numerous symptoms that frequently appear together and for which there are any number of triggers. With IBS, these symptoms tend to range from persistent abdominal bloating, cramping pain and spasming in the intestine, foul smelling wind, irregular bowel habits (bouts of diarrhoea, constipation or a combination of both) and a general feeling of discomfort in the abdominal region.
Healthy bowel function
A daily bowel movement that feels complete and easy to pass without any urgency or major effort involved indicates healthy bowel function. People with IBS rarely, if ever, experience this. Commonly they experience chronic constipation, where there is no bowel movement for many days and/or small, hard stools on an infrequent basis. This can be very uncomfortable and often results in chronic bloating and pain. As the stools are retained in the bowel toxins that the body is trying to eliminate can be reabsorbed and re-circulated throughout the body. This puts an added burden on the liver and often leads to headaches, ‘brain fog’ and general malaise.
When you HAVE to go to the toilet
Equally, an individual may have chronic diarrhoea, where a sudden urgency to relieve the bowels can occur up to 30 times a day. This is obviously distressing and often results in feelings of insecurity about leaving the house. Having loose bowels can quickly lead to dehydration, which then affects many other bodily functions. In addition, nutritional deficiencies can occur as food is not being broken down and absorbed properly. This results in feeling weak and fatigued very quickly.

Treat IBS without drugs
As there is such a diversity of symptoms and triggers are individual to the sufferer, there is no specific medical intervention to cure or even abate symptoms exists. A low fibre diet is sometimes recommended but, as I will go on to explain, this is not necessarily helpful. If the IBS triggers are not well managed, inflammation can develop within the intestine. Once this occurs any number of further factors can cause a flare-up from fatigue, an increasing range of foods and even anxiety.
Overhaul your habits to help cure IBS
Having positive, practical advice to help address IBS is essential for the sufferer's physical and emotional well-being. Such a complex condition, which has been shown to be associated with many lifestyle factors, not just diet, tends to respond really well to a more holistic approach where stress, sleep and nutrition can all be addressed together. By taking a thorough dietary and medical history, a nutritional therapist can begin to see patterns regarding specific triggers. Once these factors are addressed and better managed the internal irritation is able to calm and eventually heal, ultimately relieving the symptoms long-term and often enabling the people to resume eating foods that they once considered ‘problem’ foods.
Why the gut microbiome is important
One aspect of nutritional therapy that is an increasing focus for many clinicians is the effect of diet on the 100 trillion bacteria (known as the gut microbiome) that live in the digestive system. Long known to be involved with digestion and immune health, these bacteria have recently been shown to have a significant influence over our weight, our predisposition to chronic disease, including type 2 diabetes, our mental well-being and our ability to detoxify and eliminate carcinogens (cancer-causing substances) and even cancerous cells. They are also a big factor in the treatment of IBS.
The gut brain connection
There are many easy, daily practices that can quickly and effectively enhance the state of these highly influential gut bacteria and in turn improve inflammatory bowel problems and digestive discomfort. Anxiety, depression and other mental health problems may also be positively affected. These highly beneficial microbes, which outnumber our human cells ten to one, rely upon certain foods to thrive. Therefore, what we eat is not only feeding our human cells but also our gut microbes.
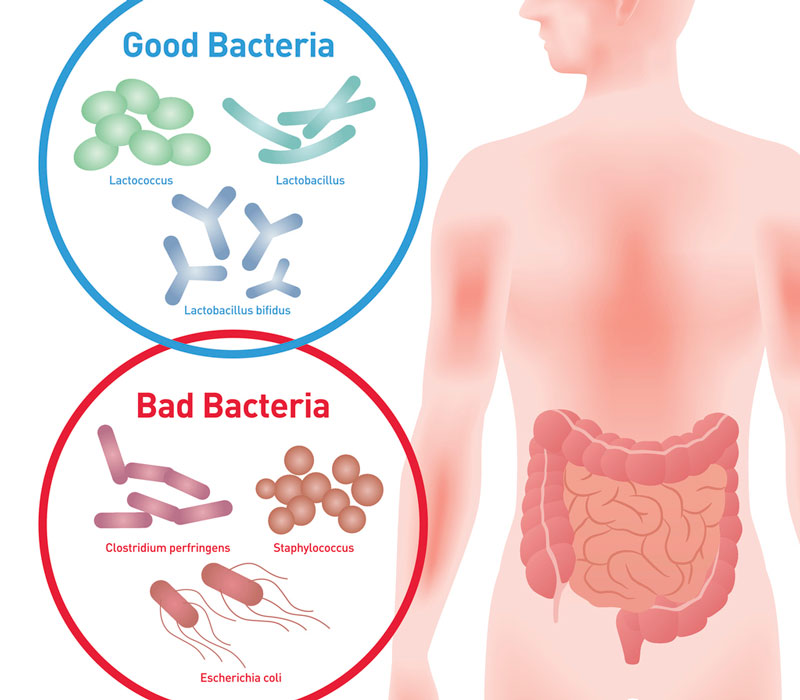
Good bacteria versus bad bacteria
As well as the trillions of really helpful bacteria other bacteria, viruses and pathogens also reside in the body and these can undermine health, especially within the digestive system. If the good bacteria outnumber the bad ones, ideally at a ratio of about four to one, then the pathogens are unable to take a hold and have any significant, negative effect on the body. However, many modern factors such as chlorine in our water, medications, diets high in refined & processed foods, artificial sweeteners to name but a few, result in the good bacteria dying off and the bad bacteria flourishing. When this gets to a critical point, inflammation and damage in the intestine occur and symptoms of IBS develop.
A bacterium, virus, or other microorganism that can cause disease.
Full medical glossaryFermented foods support healthy gut microbiome
Fermented (probiotic) foods, which contain live beneficial bacteria can help support a healthy gut microbiome by actually taking good microbes in to the gut to keep the ratio at a healthy balance. These foods include raw sauerkraut and Kimchi (fermented vegetables), live natural yogurt and kefir (fermented dairy foods), Kombucha (fermented tea) and Miso (fermented soy). Fibre, mostly found in fruit, vegetables, nuts, seeds and pulses like lentils and beans also greatly support the health of the good bacteria as they thrive on digesting fibre (prebiotic foods). Humans do not have the capacity to digest fibre, but the bacteria do it really well, allowing the good bacteria to remain healthy and grow, ensuring any bad stuff is kept at bay. This then improves our capacity to manufacture nutrients within the gut, increases the ‘intelligence’ of our immune system and improves the body’s ability to control inflammation.
Healing a damaged gut
Ironically, an initial treatment plan for IBS may involve greatly reducing fermented foods and high fibre foods as a damaged, inflamed gut that is under-functioning, with an inadequate number and variety of beneficial bacteria will struggle to cope with the addition of these live and fibrous foods, which can trigger painful bloating and acute diarrhoea. Therefore, identifying an individual’s specific triggers be it to fermented foods, all or just some raw vegetables and salad foods (raw foods take a lot of breaking down) or whether it’s onions and garlic (very common bloaters), these foods need to be avoided until the digestive system has had the chance to heal.
Getting the balance right
However, total avoidance of fermented and fibrous foods is not the answer to solving IBS, far from it. The gut bacteria need to be enhanced in number and variety to ensure good health and vitality and this can only be achieved long-term if these functional foods are included. This is where a nutritional programme to support bacterial balance and digestive robustness is essential. Using strategic dietary protocols that allow the gut to rest and heal, healthy fibrous foods and live, fermented foods can be introduced gradually to support function without triggering a flare-up.
Get help for IBS
If you are not sure if you are suffering from IBS, consider this … if you have a general awareness of your digestive system not working well or feeling uncomfortable, it is likely there is something wrong. A healthy body should digest and pass food throughout the many metres of intestine without you ever really being aware of what’s going on in there. Don’t be embarrassed and don’t suffer in silence. A dysfunctional digestive system is not something to be ignored.





