Introduction
Maintaining blood glucose levels at the optimum level is crucial to health; abnormally high or low glucose sugar levels are dangerous and if very severe can put a person into a coma. The normal healthy body copes with the daily demands by producing higher or lower amounts of insulin to either rapidly metabolise excess sugar, or reduce the rate at which it is taken from the blood. For people with diabetes, this finely controlled feedback mechanism no longer works properly, which is why measuring glucose levels becomes so important. With the internal glucose sensing system unhooked from the glucose feedback mechanism, we need to take care of that natural function for ourselves by an understanding of how we feel combined with the latest diagnostic technology.
So, what is self-monitoring, what are the tests and what is involved?
(1) Self-monitoring of blood glucose
What is this?
This is where patients check their own blood glucose level themselves using a finger-pricking device and a glucose meter. The result is displayed within a few seconds on a screen on the meter.
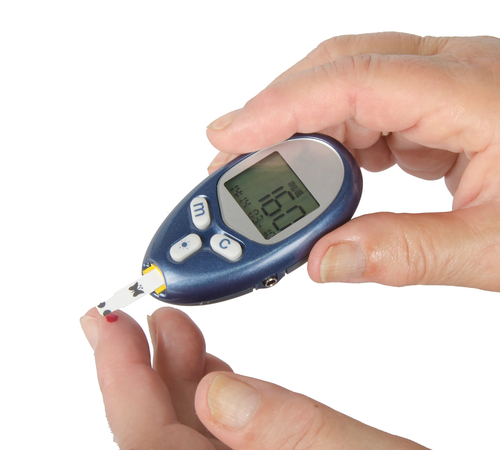
What is the point of performing self-monitoring?
Patients can’t tell what their blood glucose levels are, except when they are very high or very low. Even then, some patients can feel well despite their blood glucose having dropped to very low levels. By measuring the blood glucose they can see what the level is and act on the result. In this way, patients are able to take charge of their disease. We call this “empowering” the patient so they are in control of their own condition. Of course, the results also help the patient to know when to seek professional help.
Are there any other advantages of self-monitoring?
By looking at the pattern of results, a patient may come to understand more about their condition; what makes the glucose levels go up and down, the effects of exercise, alcohol and so on. They may get a sense of satisfaction that they are achieving good control. Indeed, if control improves as a result of self-monitoring and changes to treatment, then long term complications of diabetes may be reduced.
What about disadvantages?
Self-monitoring is not for everyone. There seems little point in measuring blood glucose levels if the patient is not going to act on them and make changes either in diet or in treatment. Just measuring the blood glucose is not, by itself, going to improve glucose control or make the patient feel better! Indeed, it may make patients more anxious or even depressed! There may be a sense of frustration or even despair when readings seem to be high or low for no obvious reason.
So who should do self-monitoring of blood glucose?
Self-monitoring is recommended for patients on insulin treatment. Patients on tablets which have the potential to cause hypoglycaemia (low blood glucose) will also benefit from performing self monitoring. Drugs such as “sulphonylureas” e.g. gliclazide, glimepiride, glibenclamide fall into this category. For other patients such as those taking metformin only, self monitoring may not be needed if other measures of glucose control (HbA1c-see below) are satisfactory. The National Institute of Clinical Excellence (NICE) has detailed recommendations on who should self-monitor. See www.nice.org.uk
Do patients get meters and testing strips on the NHS?
Patients can buy a glucose meter from a high street chemist but in fact, can usually obtain them free by directly contacting the manufacturer. Many Diabetes Centres will now supply patients with glucose meters without charge as part of their educational package. The glucose testing strips are available on prescription.
Do patients need to keep a diary with all the results?
It is good to keep a diary so that the patient and the health care professional can see the pattern of glucose results and work out what changes in treatment, if any, are needed. For example, if a patient taking insulin with meals is always experiencing very low blood glucose levels (hypoglycaemia) a few hours after the meal, this suggests either the dose of insulin is too high and needs to be reduced or the meal contains too little slow release carbohydrate. Using this information, the glucose control can then be improved. Nowadays results from most meters can be downloaded onto a computer. Some meters need connectors, others use infrared. A print-out from the computer could be used as a diary.
How often does a patient need to perform self-monitoring?
There is no fixed rule about this. For some patients, it is advisable to test first thing in the morning and during the day and at night! For example frequent testing before and after meals and at bedtime is often necessary during pregnancy or for patients on continuous insulin infusion pumps. Other patients may only need to perform 2–3 tests per day varying the timing of testing on the advice of the health professional. The relation of a test to meals is crucial. Is the test before a meal? Is it just after eating (not recommended)? Is it one hour or two hours after eating? Without knowing this information, it is very difficult to interpret a result.
What about testing at night?
In some patients there may be a suspicion that the patient’s blood glucose is dropping during the night. For example, patients wake up in the morning drenched in sweat or with headache. Sometimes the pre-breakfast glucose reading is high as a rebound from a low reading previously. This is important as it would be a mistake in that situation to increase the night time insulin dose. Patients may set their alarms and wake up in the early hours to check their blood glucose. There are now glucose monitoring systems which allow patients to sleep through the night whilst a monitor continuously measures their glucose. These devices have an implantable sensor inserted under the skin and are capable of storing 3–4 days of glucose results. These devices are usually fitted by Diabetes Nurse Specialists in the Diabetes Centre for selected patients where this information on blood glucose fluctuations at night is needed.
What about simply looking at colour changes on glucose strip instead of using a meter?
This is not advisable as it has been shown to be very unreliable. Also many of the newer testing strips do not work by colour changes and the patient can’t tell the result by looking at the strip.
Can diabetes be diagnosed using a glucose meter in someone who wants to know if they might have diabetes?
We do not recommend using glucose testing to self-diagnose. The diagnosis of diabetes has major implications for a person’s health and well-being. Whilst results from a glucose meter may be suggestive that diabetes is present, they should always be confirmed by laboratory glucose measurements.
Are all meters the same?
No - there are variations in size, size of display, weight, warranty time, memory (number of test results stored), temperature at which they operate, range of glucose measurements. Some meters are better for patients with visual impairment such as the talking blood glucose meter (BBI Healthcare). Diabetes UK has useful information for patients and health professionals at www.diabetes.org.uk
What about the finger pricking devices?
Some of the newer meters come with spring-loaded lancing devices so patients don’t need to prick their fingers separately with a lancet. Diabetes UK mentions that some patients find the FreeStyleR or FreeStyleR mini meter by Abbott Diabetes Care or the Ascensia VacculanceR lancing device by Bayer virtually painless. There is also now a laser device (the LasetteR) which produces a small drop of blood without using a steel lancet. At the time of writing this is not available on prescription and costs £495.
(2) Urine testing
Now that we have self-monitoring and glucose meters, do we really need urine testing?
As mentioned above, self monitoring of blood glucose may not be appropriate for or acceptable to all patients. Urine glucose testing may still be useful in patients with type 2 diabetes but is not usually recommended for type 1 (insulin-dependent) diabetes. Glucose doesn’t usually appear in the urine until blood levels are above 10 mmol/L so urine testing is not sensitive to smaller rises. Equally it tells you nothing about hypoglycaemia. There is also a danger that patients may become complacent if they find their urine glucose test result is always negative. Finally, older patients have a high threshold for glucose getting into the urine so they may only show positive urine glucose when the blood levels are very high. The opposite happens in pregnancy when thresholds are low and so glucose spills into the urine at much lower blood levels.
How is urine testing done?

Urine testing can be done first thing in the morning or two hours after a meal. Early morning tests are performed by emptying the bladder to discard urine passed overnight. Then a fresh urine sample is tested 30 mins later. The testing involves urinating on a test strip and comparing the colour change with the colours shown on the test strip container at the time specified by the manufacturers. The strips are available on prescription.
What about urine testing for ketones?
Do we need to go a little further with an explanation as to why ketones are indicated and therefore an additional useful marker?
Ketones are breakdown products from fat. Although a trace of ketones can appear in the urine in a healthy person who is fasting, more than + of ketones detected in the urine is abnormal and usually indicates severe lack of insulin. If the blood glucose is high (usually more than 15 mmol/L), the meter will display the message "check ketones". Ketones are tested for by strips available on prescription. All patients on insulin or who might need insulin should have strips for ketone testing.
What should a patient do if the urine test shows high levels of ketones?
This is a danger sign indicating that the diabetes is out of control. Patients should contact their doctor or diabetes specialist nurse or go to their nearest A&E or Walk-In centre.
What about urine testing for protein?
There are also test strips which detect protein in the urine as well as strips that can test for protein, glucose, ketones, and a host of other thing e.g. blood, signs of infection. Once a year, patients should have urine tested for protein as part of their annual review. If urine protein is not detected, urine samples should be checked for “albumin” which is a very sensitive marker of diabetic kidney damage. There are test strips for detecting “micro albumin” but they are expensive and most clinicians simply send an early morning urine sample to the laboratory for measurement of urine albumin expressed as the ACR (albumin: creatinine ratio).
What does a raised urine protein or raised ACR mean?
Detecting protein in the urine could indicate infection in the urinary system and the sample is usually sent to the laboratory to check for this. Some test strips may also suggest that infection is present if the urine also shows “nitrites” and “leucocytes” (white blood cells). An elevated ACR in the absence of infection is suggestive of early diabetic kidney damage (“nephropathy”). Other blood tests assessing kidney function may be required.
Can anything be done about protein in the urine?
Yes - Improving diabetic control and certain blood pressure drugs (“ACE-inhibitors”, “AR Blockers”) have been shown to reduce protein leak or stop it progressing.
(3) HbA1c testing
What is HbA1c?
This is a blood test which indicates how much of haemoglobin (the oxygen carrying red pigment in red blood cells) is “glycated” that is, affected by glucose. The higher the blood glucose the higher the proportion of haemoglobin that is glycated. The result is usually expressed as a percentage. An HbA1c below 6.5% indicates good glucose control over the previous 8–12 weeks. A high value e.g. 10% would mean that on average the blood levels have been high over the previous 2–3 months.
Why is HbA1c measured?
A blood glucose level shows the level of glucose at a particular time, for example, before breakfast. The HbA1c gives a measure of glucose control over a much longer time period-two or three months. This is useful because, of course, blood results can vary enormously over the day and what is important is that, on average, the levels are not too high. HbA1c levels show a strong correlation with complications of diabetes so that patients with values less than 6.5% have a much reduced risk of complications compared to those with high values.
What is HbA1c-IFCC?
IFCC is the International Federation of Clinical Chemistry (IFCC). This organisation has recommended changing the way laboratories report HbA1c so that laboratories around the world can compare results very easily. Instead of reporting HbA1c as a percentage, the HbA1c IFCC measurement will be in new units (mmol/mol). So for example an HbA1c of 6.5% will be equivalent to 48 mmol/mol. A conversion calculator is available on Diabetes UK website www.diabetes.org.uk As of June 09, HbA1c is now reported as both % and in mmol/mol. From 2011, only the mmol/mol value will be used.
How is HbA1c measured?
There are several different techniques used in the measurement of HbA1c but it is recommended that whatever method is used the method must be high precision and the units reported must be aligned with the results used in a major study called the DCCT. This means that the results are “DCCT-aligned” and can be interpreted in the light of the findings of that study.
Can HbA1c be used to diagnose diabetes?
No-this is not recommended. The diagnosis of diabetes is based on typical symptoms if present, and the results blood glucose measurements either fasting (7 mmol/L or more) or random (11 mmol/L or more).
How often should HbA1c be measured?
This depends whether diabetic control and treatment is stable or changing. When blood glucose levels are not yet stabilised, HbA1c may be measured every 2–6 months. The change in HbA1c rather than the absolute value is most useful during this time. Once the levels are stable, HbA1c is measured once or twice yearly.
What should the target level be?
For most people with diabetes, NICE recommends a target HbA1c below 6.5%. However targets do need to be individualised for the particular person bearing in mind the risk of hypoglycaemia, quality of life and any other factors such as co-existing medical conditions. In all cases, the patients’ views must be taken into account and the risks of high blood glucose levels balanced by the risks of the treatment.
What if the patient has very good blood glucose results from self monitoring and yet the HbA1c is high?
This means something is wrong either with the home tests or with the lab measurement of HbA1c. Various possibilities need to be explored; are the patient’s results accurate? Does the meter need changing/recalibrating? In some cases the patient is only measuring at times when the blood glucose is good (e.g. early morning or before meals) whereas the glucose concentration is high at other times (e.g. after meals) when the patient is not testing. Rarely patients have abnormal haemoglobins which interfere with the HbA1c measurement in which case the “total glycated haemoglobin” is more accurate. Advice from the laboratory or the diabetes team is needed in this situation.










