This article, by an expert in laboratory tests and screening, answers any questions you may have about drug testing and the methods involved.
Contents
- Introduction
- The testing process
- Reporting of results
- Point of Care (POC) testing devices
- The concentration of drugs in bodily fluids
- Understanding cut off concentrations
- How well do the devices perform
- Quality standards
- Health and safety
- Ensuring sample integrity
- Liaison with laboratory specialists
- In summary
Introduction
Testing for illicit drugs is often a useful tool in the clinical management of addiction, clinical toxicology, forensic toxicology and medico-legal situations for example in employment and child custody.
Drug analysis can be performed on a number of body fluids and tissues. The analytical techniques employed range from simple screening procedures suitable for use in the clinic or workplace to those requiring extensive laboratory facilities.
The testing process
Whilst most drug analysis has traditionally been based around laboratory testing of urine samples, now there is an increasing shift to preliminary screening in the clinic or workplace. Testing of oral fluid, (such as saliva) and hair has also become more widespread. It is unusual to test for drugs of abuse in blood samples.
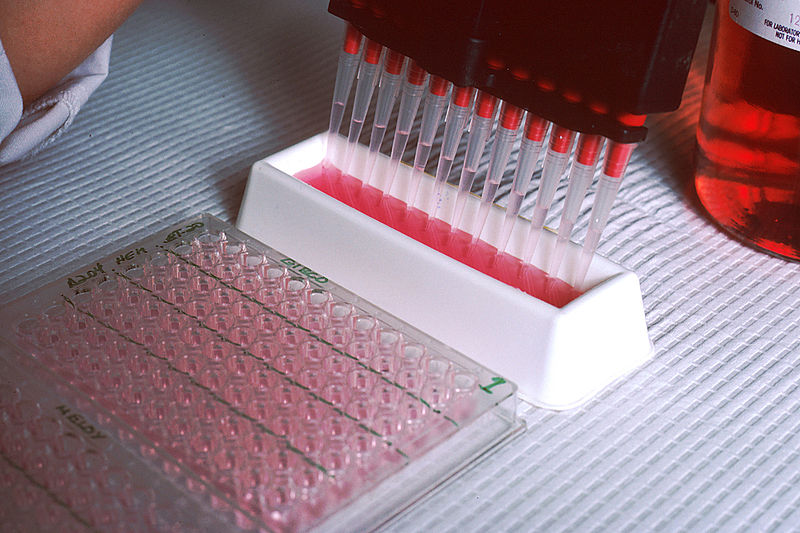
Drug tests are categorised either as screening or confirmatory procedures. Screening tests are quick sensitive methods used mainly to exclude the presence of a drug. Confirmatory tests use a different technique and chemical principle from the screening test and can identify and accurately measure the concentration of a specific drug or drug metabolite. Drugs identified as “Present” by a screening test should always be verified by a confirmatory test.
The principal classes of drugs tested in Europe are opiates (heroin, morphine, codeine and dihydrocodeine), cocaine, amphetamines (including “ecstasy”), barbiturates, benzodiazepines, and cannabinoids. Other drugs which may require testing include methadone, phencyclidine (PCP), buprenorphine, dipipanone, the piperazines, blocking drugs, antihistamines, decongestants, laxatives and diuretics. In any drug testing setting it is important to define which drugs are legitimate and which are not. Agencies involved in testing must have clear guidelines on which drugs will be tested and how the results will be applied.
Drug availability and patterns of use vary on a geographical and social basis, and consultation with local laboratory and addiction agencies can often help to identify which drugs are most appropriate to test for.
Reporting of results
To avoid confusion of results it is best practice to avoid the use of the terms “positive” and “negative”, when referring to the drug testing results. The terms “Present” and “Not found” are less susceptible to misinterpretation.
Traditionally testing of biological samples for illicit drugs has been left to specialised laboratories. The advent of immunoassay technology has enabled tests to be performed outside the laboratory, either using small desktop and hand held analysers or by the use of visually read stick, slide or cup devices.
Point of Care (POC) testing devices
An increasing range of substances can now be measured using POC devices and most common drugs of abuse can be detected using them. The devices generally rely upon the principle of immunoassay which uses antibodies to bind the drug under investigation in the sample.
It is important to appreciate that antibodies bind a range of substances within a class of drugs.
They therefore can be considered to detect classes of drugs rather than identifying a specific drug. For example; a POC test for opiates is likely to detect codeine, morphine and dihydrocodeine, therefore it does not enable differentiation between heroin abuse and use of a legitimate pain killer. Thus POC testing devices are considered to have a low specificity for an individual drug. The use of the immunoassay principle does however mean that the devices are able to detect very small amounts of a substance (high sensitivity). So a test that shows a drug is “Not found” has a good probability that the drug is not “Present”.
The sample is applied either by dipping the device into the urine sample or by applying a few drops of urine to a slide using a pipette. The sample diffuses through a wicking support and interacts with antibodies to develop or inhibit the formation of a colour. It is essential to establish, prior to use, whether a drug is to be shown to be “Present” by absence or formation of colour. Mis-reading of results is very common and it is vital therefore that there is adequate training before the devices are used.
The primary advantage of these POC devices is the ability to produce a result within a few minutes while the subject is still in the clinic or office. This can speed the decision making process and may lead to more effective management.
The concentration of drugs in body fluids
The amount of drug in a sample of urine or saliva will be influenced by many factors. These include the size of the dose taken, the rate of metabolism and rates of urine production (or saliva flow). Following ingestion of a drug the concentration in the urine (or saliva) will firstly rise and then fall over a period that may vary from a few hours to a few weeks. Some drugs such as LSD or the short acting benzodiazepines may only be detectable for a few hours, while other drugs such as cannabis may be detectable for several days or weeks depending on the extent of use.
Understanding cut off concentrations
These devices cannot be adjusted in any way and have a fixed cut-off point. They are designed by the manufacturer to show the presence of a drug above a fixed concentration.
Manufacturers vary as to which cut off is used. For example a urine test for opiates from one supplier may have a designated cut off of 300 ng/mL while others may have cut off points of between 20 ng/mL and 2000 ng/mL. Devices set to 300 ng/mL for opiates may be appropriate to establish that no drugs have been consumed but they are likely to give a result of “Opiates “Present”” when a subject has consumed poppy seed containing foods or when a habitual heroin user has been abstinent for a couple of weeks. Therefore the choice of devices can lead to misinterpretation of results and it is essential that the device employed matches the purpose of the test.
Guidelines exist for the appropriate cut off concentrations to be used in workplace and clinical settings.
Laboratory based procedures are normally quantitative and so the cut offs used can be varied according to the setting of the test. Importantly this also allows for serial monitoring of samples, so when a drug is “Present” it is possible to show if the concentration is falling over time.
How well do the devices perform
An MHRA Evaluation Report examined sixteen point of care testing (POCT) devices available in the UK for the detection of drugs of abuse in urine. The devices tested included both single and multiple test devices.
The report highlighted the same specificity issues that are inherent with all antibody based procedures as well as issues particularly associated with POCT devices:
- Interferences particularly of note were the over-the-counter preparations: Boots poppy seed bar, codeine linctus and pholcodine interfering with the opiates and morphine devices; Nytol with some methadone devices and occasionally Ranitidine and Ibuprofen with other devices.
- Problems of misinterpretation due to the inherent use of reverse logic in most devices.
- Manufacturers’ batch-to-batch variation in production and the subjective interpretation of the presence or absence of a colour led to a large variability in the reporting of results particularly when the concentration of a drug was close to its cut-off
- Manufacturers’ product variability led to a relatively high device failure rate.
Since this report was written the standard of devices has certainly improved, however all the points above about the performance of these devices remain genuine concerns.
Quality standards
The use of such devices within a clinic or workplace pose particular challenges to accurate record keeping and quality assurance, which are much more closely controlled in a laboratory environment.
Quality assurance forms an integral part of the testing process. Clinical and forensic laboratories work to established quality standards that cover all aspects of the testing process, from the collection of the sample through to the comments that appear on the final report. In the laboratory internal control samples will be run frequently to ensure repeatability of results. Accredited laboratories also participate in external quality assurance schemes where ‘blind’ samples are analysed and reported to the scheme organiser. Poor performance in such schemes can ultimately lead to loss of accreditation.
Accreditation of health care environments using POC testing is likely to become a mandatory requirement in the near future.
Users of POC devices should also run quality control samples to ensure reproducible results. Many devices include a second band in the testing strip. Although this shows that the sample has been applied correctly, it does not show that the drug result is correct. Quality control samples are commercially available at a range of concentrations. Regular testing of a sample that has a drug concentration within 30% of the defined cut off will help to provide evidence of repeatable results. The frequency of checking will depend on the number of tests performed and the number of operators of the tests. Checking weekly using different operators is a reasonable minimum frequency. Quality control samples should always be run when a new batch or lot number of devices is started.
The provision of appropriate documentation is an important part of the testing process. This is required to enable retrospective review of results and to cross check information when results are challenged. Just recording results in patient notes is inadequate for this purpose. Lot/batch numbers of reagents or test strips must be recorded together with quality control data.
Health and safety
Good Health and Safety procedures are most important in the handling of all biological fluids. Unsealed urine and saliva samples pose a significant risk of infection. It is essential to provide a suitable area, away from office papers or food, to perform the tests. This should be a contained area, with suitable benching and floor covering. Suitable waste disposal facilities are a legal requirement.
If samples are to be sent for confirmatory testing to a reference laboratory then appropriate refrigerated storage must be available and sample transport must conform to national legal standards.
Ensuring sample integrity
The nature of drug use requires that comprehensive measures be in place to ensure the integrity of each sample. This is both to avoid cheating on the part of the subject but also to protect the testing employer and agency against accusations of unfairness. The UK Workplace Drug Testing Guidelines give extensive advice on the procedures required and should be consulted for particular details whilst the general headings are given below:
- That the subject providing the sample is the correct individual undergoing the test.
- The sample collection procedure should protect the dignity and human rights of the subject.
- Sample collection should be conducted by suitably trained personnel (the collecting officer). The security of the premises designated for the procedure must be adequate and only named personnel granted access.
- The collection officer must adopt procedures to minimize the risk of adulteration of the sample either by the subject, the person supervising the collection or a third party.
- To deter tampering of the sample, the collection officer will check for any concealed substitute samples, water containers etc. All taps in the WC must be sealed or closed off and the toilet water coloured with a bright blue vegetable dye.
- Access to any chemicals (soap, bleach etc) which may adulterate the sample must be prevented.
- The sample containers should be clearly identified with a unique identifier from the time of collection through to the time of disposal following any period of post analytical storage
- Suitable records must accompany the entire process recording each stage from sample collection, transportation, analysis, storage and disposal. to issuing of results.
Liaison with laboratory specialists
Regular liaison between laboratory specialists and clinical staff is crucial if drug testing is to be used effectively.
Clinical staff may be unaware of the physiological or pharacokinetic absorption, metabolism and excretion factors that influence a “Present” of “Not found” result. The principles of detection limits, sensitivity and specificity are often challenged by employees or patients and are best referred to laboratory personnel who can authoritatively deal with such questions.
Drug testing when child custody is involved is particularly sensitive and should always be referred to a specialist laboratory where confirmatory techniques are available.
In summary
POC testing often fails when staff are not regularly trained and re-trained. A regular programme of training is essential to achieving reliable results, this must include provision for training locum and bank staff.
The finding of drug “Present” results, especially for opiates and amphetamines, requires confirmation. These samples must then be transported to a reference laboratory for further tests. Within the drug addiction culture, urine test results are frequently challenged. Initially this may require the re-testing of occasional samples. However, further tests may be requested after subsequent interviews with the patient. Samples will need to be stored for between 3 and 14 days in a secure refrigerated unit. Where a legal challenge is likely then secure storage under chain of custody is necessary.
POC tests are not quantitative and offer no indication of the amount of drug in a sample. Laboratory procedures are at least semi-quantitative and may determine the actual amount of drug even if this is not routinely reported.
The provision of appropriate documentation is an important part of the testing process. This is required to enable retrospective review of results and to cross check information when results are challenged. Just recording results in patient notes is inadequate for this purpose.
Maintaining sample integrity is one of the difficulties of all drug testing. Drug users are always imaginative in attempts to “beat the tester”. A range of laboratory procedures are used to check urine samples. These are not available for the POC testing, but provision must be made for them to be performed.
Close liaison with reference laboratories is essential for appropriate confirmation and interpretation of results.
If you would like to have more information on testing, or have a question please complete our simple online form
References
Defining a limit of detection and limit of quatitation as applied to drug of abuse testing: (Editorial Comment)
Lawson GM Clin Chem, 1994 Jul, 40.7 Pt 1, 1218-9
Accuracy of five on-site immunoassay drugs-of-abuse testing devices
Taylor EH; Oerti EH; Wolfgang JW; Mueller E J Anan Toxicol, 1999 Mar, 23:2. 119-24
Laboratory tests for rapid screening of drugs of abuse in the workplace: a review.
Schwatz RH; Clark HW; Meek PS J Addict Dis, 1993 12:2,43-56
United Kingdom Laboratory Guidelines for Legally Defensible Workplace Drug Testing. Version 1 March 2001.
http://www.wdtforum.org.uk
Laboratory Screening for drugs of Abuse.
S. George. Rila PublicationsLtd. CPD Bulletin Clinical Biochemistry,1999;3: 85-90
Sixteen devices for the detection of drugs of abuse in urine. Medicines and Healthcare products Regulatory Agency, MHRA 03078, 2003










