The NHS Breast Screening Programme provides free breast screening every 3 years for all women aged over 50 years. This article provides answers to the key questions that you may ask when you are invited to be screened.
Contents
- What are the facts about breast screening?
- What is a mammogram?
- Does breast screening really work?
- Problems with mammographic screening
- Does screening lead to unnecessary treatment?
- The benefits of surgery
- Unnecessary anxiety over abnormal mammograms
- Recommended breast screening for other ages
What are the facts about breast screening?
Screening for breast cancer should be particularly effective because it is one of those cancers where catching it at an early stage makes a huge difference to the chance of cure. There are a number of reasons why the survival rates from breast cancer have improved steadily over the last thirty years, but it is thought that the most important factor has been early diagnosis. Routine breast screening is fairly well established in many countries, but there has been recent controversy regarding its benefits.
All types of medical screening have their drawbacks including missed diagnoses, further investigations that turn out to be unnecessary, anxiety caused by recalls, and treatment for conditions that would not have caused any problems if they had been left alone. For breast cancer the only type of screening that has proven to be effective is regular routine mammography. A mammogram is a breast x-ray so an additional problem with this type of screening is the exposure to radiation. However, breast cancer is a major health problem and an effective form of screening is very desirable. It is the most common type of cancer that affects women, with one in nine females in the UK being diagnosed with the problem during their lifetime.
What is a mammogram?
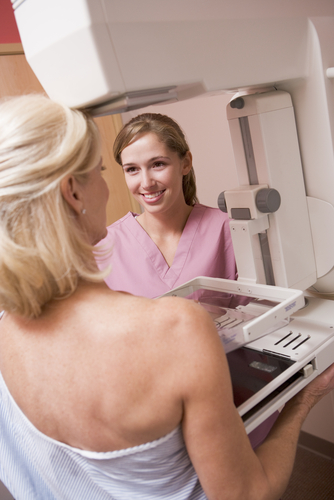
A mammogram is a simple x-ray of the breast tissue. It is carried out by gently compressing the breast between two plastic plates while standing in front of the x-ray machine. Usually two x-rays are taken of each breast, one from side to side and one from top to bottom, giving four mammograms in total. For the purposes of screening sometimes only one oblique mammogram is done on each side. In the last two or three years mammogram machines have been designed that work on digital technology. Just like a digital camera, the picture is an electronic file and can be magnified up and altered in contrast, which can be an aid to diagnosis. Most women do not find a mammogram too uncomfortable, but it can be painful particularly if you have tender breasts. The signs of breast cancer on a mammogram include a localised (dense) lump, distortion of the internal architecture of the breast, and some types of calcium deposition.
The NHS Breast Screening Service is one of the best in the world. It has very high standards that have been consistently maintained throughout the country. Breast screening starts at the age of fifty and comprises a regular mammogram carried out every three years. Although the NHS Breast Screening Services stops sending out regular appointments after the age of seventy, you are entitled to contact them yourself on a three yearly basis after the age of seventy to continue with screening. Currently the NHS Breast Screening Service carries out a two view mammogram on the first visit and single view mammograms thereafter. Most screening is still done using analogue equipment, but there are plans to change over to digital and also to do two views at every screen, both of which will lead to more accuracy.
Does breast screening really work?
The statistics from breast screening programmes around the world have shown that having a regular mammogram catches breast cancer at an earlier stage and definitely results in higher cure rates. In addition, mammograms can identify pre-cancerous changes, which if dealt with promptly usually prevent the development of breast cancer altogether. The NHS Breast Screening Service screens approximately two million women every year. Approximately 14 thousand cancers are diagnosed and currently statistics show that nearly three thousand lives are saved every year.
Problems with mammographic screening
One of the problems with screening using mammography is the exposure to radiation. X-rays are harmful and do contribute to the causes of breast cancer. For mammography the radiation dose is fairly low and is less than most types of medical X-ray. You would receive a similar amount of radiation from the atmosphere if you flew to Australia and back, for example (you are exposed to high levels of cosmic radiation at high altitudes). X-rays are more damaging in younger women, which is one reason why we tend not to do mammograms under the age of 35. Studies have been done to try and estimate the likelihood of regular mammograms causing breast cancer. The estimates for the NHS breast screening programme are that radiation from mammograms causes sixty new cancers a year and that there would be approximately twenty deaths as a consequence. This figure of twenty deaths has to be compared with the figure of nearly three thousand lives saved by the early diagnosis of breast cancer. At the end of the day the benefit to risk ratio of screening mammography can best be judged by looking at the results of breast screening programmes in many different countries. The statistics clearly show that women who have regular mammograms as part of the breast screening programme have a considerably lower risk of dying of breast cancer, so clearly the practical benefits do definitely outweigh the dangers of the radiation.
Does screening lead to unnecessary treatment?
Recently the newspapers have carried stories of unnecessary surgery and even mastectomy resulting from breast screening. In the NHS 8 out of every 9 surgical diagnostic biopsies confirms breast cancer meaning that few women undergo unnecessary biopsies. There is however more concern that some conditions for which surgery is recommended may not have caused any significant problems during the rest of the individual woman's life if they had been merely left alone. Undoubtedly there are a small number of cancers that do not progress as expected. The best estimates are that 93% of invasive cancers would be fatal if left and around 7% may never cause any harm. Unfortunately our current diagnostic tests do not allow us to decide which is which.
The benefits of surgery
Given the choice most women would choose to have treatment rather than hope that they are one of the small number of women with harmless cancers. There is perhaps more of a problem with the diagnosis of pre-cancerous changes (DCIS, ductal carcinoma in-situ). DCIS is a precursor to invasive cancer, but in its own right is entirely harmless. If removed by surgery, the development of the invasive breast cancer can often be avoided. There is concern that some cases of DCIS never progress further to invasive breast cancer and therefore surgical removal is an unnecessary treatment. In fact more than 60% of cases of DCIS diagnosed at breast screening are termed high grade. This type of DCIS always turns in to breast cancer and when it does it results in an especialy aggressive type of breast cancer. The detection of high grade DCIS is therefore particularly valuable and prevents many women from developing breast cancer and requiring more extensive treatments such as chemotherapy. Less frequently intermediate and low grade DCIS are diagnosed at breast screening. Intermediate grade DCIS will usually also turn in to breast cancer eventually and surgical removal is therefore definitely beneficial. The main problem is with low grade DCIS. This probably only turns in to breast cancer in about a third of cases, meaning that surgery to remove it is excessive in more than half of women. However, low grade DCIS is the least commonly diagnosed type of DCIS at breast screening. If the problem is localised to a small area of the breast, a simple day case operation can remove it completely and is surely worthwhile. There are only a few occasions where the low grade DCIS is very extensive requiring a mastectomy as the only way of removing it all. This situation is certainly controversial and presents difficult decisions. The statistics and chances of cancer development are always carefully explained to patients with DCIS. In fact, in my experience, most women given a one third chance of developing breast cancer in the future opt for surgery and sometimes even mastectomy. In a well informed screening service these difficult situations are discussed with women at length and women can then make their own choice.
Unnecessary anxiety over abnormal mammograms
The other obvious problem with breast screening is the considerable anxiety that is generated by being called back for further investigations. In the NHS approximately one in twenty women having a mammogram are called back. Many of these do not have cancer and it is unfortunate that women have a very worrying time until further tests have been completed and the results come through. You might say that this is the price that you have to pay for an effective breast screening programme that undoubtedly saves thousands of lives per year. The NHS screens 2 million women a year and although they have cut down the waiting times it would be very difficult to get round this problem. If you are found to have an abnormal mammogram it is possible to take the films to a private one-stop diagnostic clinic where the abnormalities can be assessed and usually immediately resolved. Some private hospitals and clinics, such as The Harley Street Breast Clinic, will even do routine screening within a One Stop diagnostic clinic where the results are immediately available and any abnormalities can be sorted out right away.
Recommended breast screening for other ages
In most countries routine screening mammograms are carried out every one or two years. The current interval of a mammogram every three years for women between the age of fifty and seventy as practised by the NHS is not optimal but nonetheless it is still very effective and saves thousands of lives each year. A mammogram done every one to two years will give the best protection against breast cancer, but in the UK this has to be done privately. Some women arrange to have an additional mammogram half way between each NHS screen.
Breast cancer is common between the age of forty and fifty and in other countries mammographic screening has been shown to be effective in this age group as well as the fifty to seventy age group. However, younger women more often develop more aggressive and faster growing cancers and effective screening therefore requires a mammogram to be carried out more frequently. The ideal is to have a mammogram on an annual basis between the age of forty and fifty. Under the age of forty breast cancer is less common and the effect of radiation is a little more damaging. In this age group mammograms are also much less effective at diagnosing breast cancer. Between the ages of thirty and forty, therefore, if a woman wants to be screened an annual ultrasound scan is usually better than a mammogram. Over the age of seventy, breast cancer becomes more common than in any of the younger age groups. It is therefore still very important to have regular breast screening with regular mammograms carried out every two to three years. In the UK the NHS provides effective breast screening and all you have to do is to attend for the appointments that will be automatically sent to you between the ages of 50 and 70. Additional breast cancer screening outside this age group needs to be a personal choice and be privately funded. Mammograms are not too expensive, costing between £140 and £220 depending on the sophistication of the x-ray machine and the quality of the reporting, so it is a choice that most women can have.










