This article describes the common condition of male breasts also known as gynaecomastia. This will be of help to any man who may be suffering from gynaecomastia and would like to know whether to go ahead with treatment.
Contents
Introduction
Gynaecomastia, in simple terms means abnormally large breasts on men and derives from the Greek ‘gyne’ meaning women and ‘mastos’ meaning breasts. The condition is relatively common and affects approximately 40% of men. Gynaecomastia, also known as man boobs or ‘moobs’ can cause feelings of shame, self-hate, inadequacy and sufficient embarrassment to interfere with a patient's social life.
The causes of gynaecomastia
Idiopathic
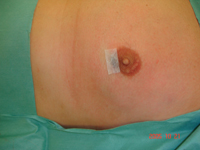
Idiopathic gynaecomastia, is spontaneous and the cause is unknown. This is the most common type of gynaecomastia, of which the majority of cases are due to puberty.
Approximately half of all adolescent boys will experience gynaecomastia as the breast buds develop due to changing hormones during puberty. This can be due to a lack of androgen, or an overabundance of oestrogen. This will normally be temporary, becoming most prevalent around the age of 14 and will resolve by itself, not requiring treatment.
Drugs
It is thought that about 20% of cases of gynaecomastia are a result of chemicals or hormones found in drugs taken either for either medical or recreational reasons.
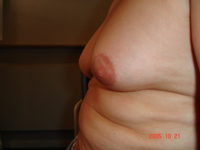
Anabolic steroids typically used by body builders can cause glandular gynaecomastia whereby the tissue underneath and surrounding the nipple becomes concentrated and enlarged causing the appearance of a ‘puffy nipple’. This results from the excess levels of testosterone found in the steroids which, when converted to oestrogen, will cause breast growth.
Gynaecomastia has been associated with medications such as antidepressants, anti-psychotics, oestrogens (for prostate cancer), cimetidine (for heart burn and peptic ulcers), digoxin (for heart flutters) and spironolactone (for heart failure).
Social drugs such as alcohol, amphetamines, heroin and marijuana have been found to correlate with gynaecomastia although there is disputed evidence as to whether they can cause the condition. When a patient is seen by the consultant, a thorough history is taken and asks about past and present drug use.
Obesity
Gynaecomastia occurring as a result of obesity is a result of an excess of adipose tissue. Fat on the chest giving the appearance of breasts without growth of the glandular tissue is known as pseudogynaecomastia and is therefore closely related to exercise and diet.
Chronic liver disease
As the liver is responsible for detoxification, biochemical production and hormone production, any problems with the liver will lead to a disturbance of these factors. The hormones involved in problems with the liver, as well as the medication for cirrhosis of the liver are known to cause gynaecomastia. Cirrhosis of the liver will lead to increased oestrogen production which, in turn, can increase growth of the breast tissues.
Thyroid problems
Similarly to the liver, when there are problems with the thyroid gland this leads to an excess of certain hormones which can lead to breast growth in men.
Kidney disease
During kidney disease, the hormonal balance in the body is disrupted which, as in hyperthyroidism or liver disease, can lead to gynaecomastia. About 50% of people suffering from kidney failure and receiving haemodialysis will experience the condition.
Klinefelter syndrome
Klinefelter syndrome is a genetic condition whereby a man is born with at least one extra X chromosome (normal males have one X and one Y chromosome). Approximately one in every 500–800 males are born with the condition which is signified by low testosterones resulting in small testicles at puberty and infertility. Around a third of men with Klinefelter syndrome will also suffer from gynaecomastia.
Other causes
- Genetics
- Cancer of the breast and testicles (this is rare)
- Testicular insufficiency
Gynaecomastia treatment
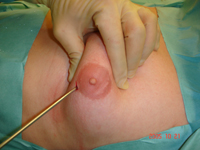
The patient should be seen by a breast specialist in order to identify the potential cause and exclude sinister conditions such as breast and testicular cancer.
Non-surgical treatment
Gynaecomastia in teenage boys tends to resolve by itself in around 90% of cases over a one–two year period.
If the condition is causing sufficient embarrassment to interfere with the patient's social life, then the cause if identified should be removed or the underlying medical condition should be treated.
Painful gynaecomastia may be treated successfully with tamoxifen (10 mg per day), an antagonist of the oestrogen receptor responsible for the growth of cancerous cells.
Drug-induced gynecomastia resolves when the drug causing the condition is stopped, similarly, pseudogynaecomastia can be limited by controlling diet and increasing exercise.
Surgical treatment

Surgical correction remains the most effective treatment of symptomatic gynaecomastia. The best surgical technique involves a combination of surgical excision of the glandular component and liposuction of the fatty component using small incisions around the areola below the nipple leading to an almost invisible scar. The excessive skin tends to shrink over time. I recommend the avoidance (if possible) of techniques which involve removal of excessive skin and free transfer of nipples in view of the inferior cosmetic results associated with these techniques.
Liposuction alone (under local anaesthesia and sedation) is effective for pseudogynaecomastia (gynaecomastia due to excessive fatty tissue in the breasts).
Post-operative follow-up
The patient is usually seen once in the clinic for a wound review after the operation. Some patients develop fluid accumulation at the site of surgery called seroma; this is usually self-limiting but may require fine needle aspiration. Some patients may require psychological counselling.

