This article by Dr Nigel Hacking updates a very promising new treatment for benign prostatic hyperplasia (BPH) called Prostate Artery Embolisation. This emerging therapy will be of particular interest to men who have previously received medical or even surgical treatment for this condition that has not proved successful.
Contents - Prostate Artery Embolisation for BPH
- Introduction to benign prostatic hyperplasia
- Symptoms of BPH
- Treatment of BPH
- Trans Arterial Embolisation
- Prostate Artery Embolisation
Introduction to benign prostatic hyperplasia
Benign prostatic hyperplasia (BPH) is the condition that occurs when the prostate gland is increasing in size without there being any malignant cause. As the prostate enlarges it leads to compression and then obstruction of the urethra, which in turn affects urinary flow. The symptoms include urinary frequency, urinary urgency, hesitancy in urination, poor stream and incomplete bladder emptying. Partial obstruction can ultimately become complete causing acute urinary retention and the urgent requirement for a bladder catheter. BPH is not however a pre-malignant condition.
This condition becomes increasingly common with age and has an impact on the quality of life for a considerable number of men aged over fifty years.
Traditionally, BPH has been managed with lifestyle changes and medication in the first instance but if the symptoms progress or become severe then surgery may be required. However, as this is an age-related condition fitness and suitability for surgery is often an issue. The process by which the prostate begins enlarging starts around the age of 30 and up to 50% of men will show histological signs (changes within the tissues) of BPH by 50 years of age. By 80 years of age this rises to 75% although not all of these men will have symptoms. Symptomatic BPH occurs in up to 50% of men of middle age or older.
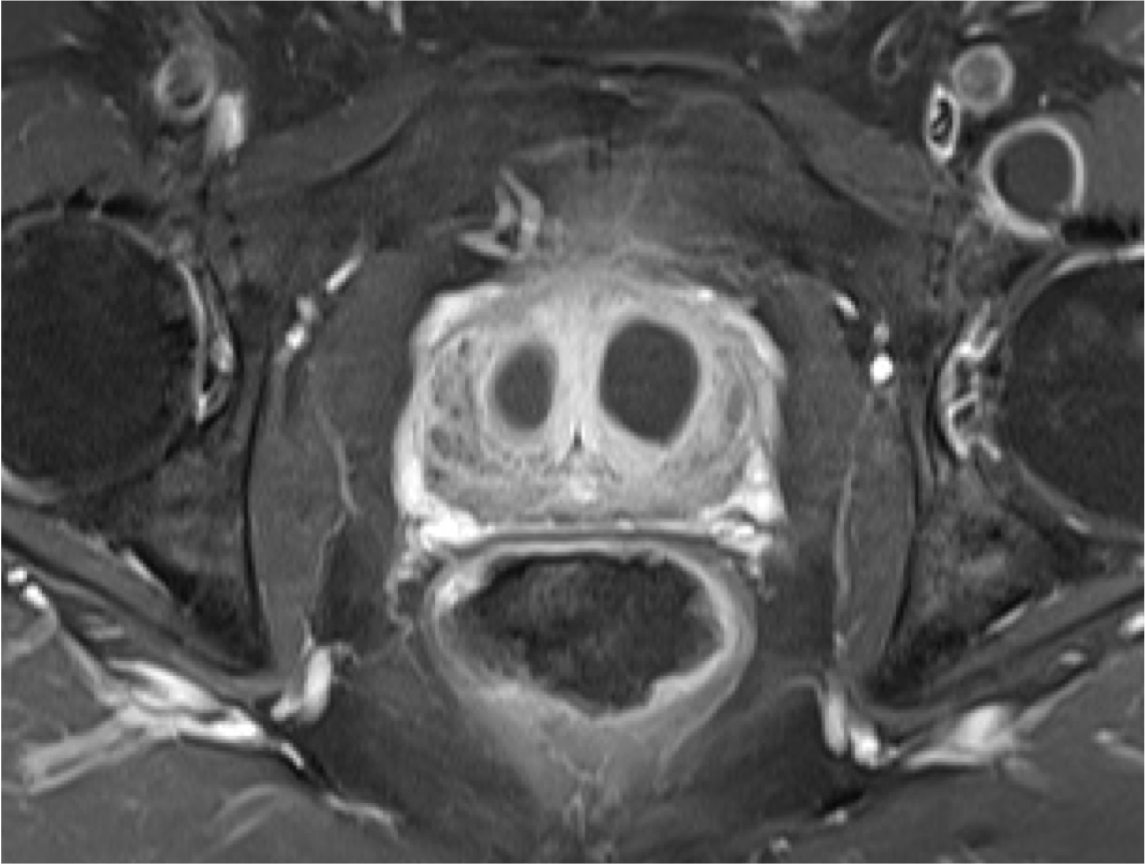
Post PAE contrast enhanced MRI scan shows that the troublesome central 'adenoma' or benign growth causing the symptoms has become devascularized or lost its blood supply. This leads to gland shrinkage and an improvement in urinary flow and a reduction in night and day time urinary frequency
Symptoms of BPH
The symptoms of BPH fall into two broad categories
- Voiding (weak stream, hesitancy, stop and start micturition)
- Storage (frequency, urgency, nocturia, leaking)
Treatment of BPH
Both of the sets of symptoms set out above occur in BPH. The management of BPH varies according to the nature and severity of the symptoms. Lifestyle changes and medication (such as the drugs known as alpha blockers and 5ɑ-reductase inhibitors) are used initially, but if symptoms progress despite conservative therapy then surgery may well be suggested.
There are a number of different forms of surgery that will typically be offered depending on the size of the prostate gland including Trans Urethral Prostatectomy (TURP) or Open Prostatectomy. However, minimally invasive thermal ablation using microwave energy (TUMT), radiofrequency (RF), laser energy (PVP, HoLAP/HoLEP) and the Urolift procedure have not yet gained widespread usage.
Trans Arterial Embolisation
Trans-arterial embolisation, a non-surgical, minimally invasive procedure, has been used in many clinical settings. Initially introduced to stem life-threatening haemorrhage it then evolved into more widespread use to block the blood vessels that serve tumours prior to surgery and then again for definitive palliative treatment of tumours. It has been used in the setting of prostatic disease for many years either to stem acute or chronic bleeding due to advanced prostatic cancer, but also to control bleeding after prostatic surgery or even biopsy.
Uterine Artery Embolisation in the treatment of women with uterine fibroids, has become one of the most common minimally invasive treatments for symptomatic fibroids in the UK and is fully recognised by NICE (National Institute for Health and Clinical Excellence).
Prostate Artery Embolisation
Prostate artery embolisation (PAE) has been the subject of several studies since 2010, notably from Sao Paulo, Brazil, Lisbon, Portugal, China and the UK. The groups have been testing the hypothesis that trans-arterial embolisation of the prostate could lead to the death of the blood-rich and overgrown prostatic tissue, which in turn would result in a subsequent reduction in obstructive urinary symptoms.
Several Randomised Controlled Trials (RCTs) have now been published and in 2017 Pisco presented the results of his 1000 patient study at the Society of Interventional Radiology (SIR) meeting in Miami. This series includes the longest follow up data with over 800 patients followed out to 3 years and over 400 followed beyond 3 years.
As in all published PAE series to date symptomatic improvement is seen in just over 80% of men at 3-12 months and these improvements are sustained at medium and long term follow up with cumulative success rate of 78%.
The UK-ROPE (Registry of Prostate Embolisation), sponsored by NICE as well as the National Professional Societies of both Interventional Radiology (BSIR) and Urology (BAUS) performed between 2014 and 2016 will report it’s 1 year results in mid 2017.
One Hour Procedure for BPH
The procedure is performed by trained Interventional Radiologists who are experienced in advanced embolisation techniques. It typically involves a unilateral groin puncture, under local anaesthetic and then thin, hollow tubes known as catheters, are placed into both right and left prostate arteries under direct X-Ray guidance. These prostatic arteries are then closed using 100-500 micron-sized embolic particles. The procedure takes approximately 1-2 hours to perform and the patient can be discharged after 4 hours provided he is fit. Men needing to travel out of the area or those who are less fit may require an overnight stay in hospital.
Post-procedural pain is usually mild to moderate, unlike the often severe post-procedural pain following fibroid and kidney embolisation. This discomfort can be managed by simple anti- inflammatory and pain killing oral medications.
Potential Complications
Complications reported to date have been rare and mostly involve minor bruising of the groin. One case of non-target embolisation of the bladder and several minor self-limiting ulcerations to the rectum have been reported in over 2000 cases; of these, one required surgical bladder repair. Minor again self- limiting penile ulceration has been reported in small numbers.
It is encouraging that the common side effects of TURP, such as transient incontinence, erectile dysfunction and particularly retrograde ejaculation have not been reported.
Southampton Experience
A carefully Monitored Clinical Introduction in 25 men with proven and symptomatic BPH, not responding to medical treatment was instigated at Southampton University Hospitals in 2012. The procedure was technically successful in all patients’ and clinical improvement, although in some cases modest was been seen in 90%. There were no serious complications and post procedural pain was mild to moderate only. In all but exceptional cases these were performed as a day case procedure.
NICE considered PAE as an option for treating men with significant Lower Urinary Tract Symptoms (LUTS) caused by benign prostate enlargement in 2013 and decided that at that time the evidence was still not strong enough to recommend approval for PAE. They suggested that more studies were needed and that included the setting up of a National Registry comparing PAE with traditional surgical techniques using TURP or HoLEP.
Dr Nigel Hacking, as the Pioneer of PAE in the UK, was appointed as Chairman of the UK-ROPE Steering committee and it’s Clinical Lead. Over 300 patients were recruited into UK-ROPE from 18 centres’ between 2014 and its close in early 2016. 1-year follow up data was completed in early 2017 and outcome data is being analysed and will be available later in 2017.
There were no serious concerns over safety of the PAE procedure.
To date Dr Nigel Hacking and his team at Southampton University have performed over 200 PAE cases with excellent results. A few patients have shown early symptom recurrence at 3-12 months and have undergone a limited TURP to remove an enlarged ‘Median lobe’. This limited surgery can still avoid the side effects seen after full TURP and this 2-stage procedure may be helpful in some cases.
NICE is likely to reconsider PAE later in 2017 or 2018 once the UK-ROPE report is complete and they will also look at the latest studies published from around the world since 2013.
Dr Hacking is planning to be the Chief Investigator and Clinical Lead for a European or Global Registry of PAE commencing in 2018, aiming to recruit 1000 PAE cases, using the same multi-disciplinary approach as was used in UK-ROPE.
For a private PAE referral
A GP or Urology referral will be required and arranged by Dr Hacking, and a full assessment with both Urological and Radiological assessment will be required before PAE can be offered.
For further information on the author of this article, Consultant Radiologist, Dr Nigel Hacking, please click here.
Inability to maintain a penile erection for sexual intercourse, also referred to as impotence.
Full medical glossary

