Consultant Orthopaedic Surgeon Andrew Sankey specialises in conditions affecting the shoulder. Here he describes the treatment options for osteoarthritis of the shoulder and other degenerative or traumatic shoulder complaints.
Treating osteoarthritis in the shoulder
- What is osteoarthritis of the shoulder?
- Symptoms of osteoarthritis of the shoulder
- Diagnosing shoulder complaints
- Non-surgical treatment of shoulder problems
- Arthroplasty or joint replacement surgery for shoulder problems
- What special circumstances affect shoulder replacement surgery?
What is osteoarthritis of the shoulder?
Most People are very familiar with the idea of joint replacement surgery for the hip and knee but perhaps less so with shoulder replacement. However, osteoarthritis does affect the shoulder joint too and sometimes shoulder replacement surgery becomes necessary.
Osteoarthritis is a degenerative condition of the joints that develops gradually over many years for and often for no obvious reason. Occasionally it may be associated with injury, such as multiple shoulder dislocations or a fracture involving the head of the humerus (ball) or glenoid (socket). The protective cartilage of the joint wears away, leaving bare patches of bone that rub against each other. There is a large genetic component to developing osteoarthritis, and therefore it need not be related to sport, activity or occupation.
Symptoms of osteoarthritis of the shoulder
Pain and stiffness are the most common symptoms of osteoarthritis, and they often develop gradually over months or years. The pain is aching in nature and situated over the front and back of the joint, and also down the outer aspect of the upper arm, even radiating towards the elbow. It may be worse in cold or damp weather, and may cause sleepless nights. Activity makes the pain worse.
Stiffness is due to the joint surfaces becoming uneven and a high degree of friction between the bare bone of the opposing joint surfaces. Movement may cause a ‘creak’ that may even be audible. Functional ability may be limited by being unable to reach behind one’s back, to reach a pocket or fasten a bra, or to raise the arm high enough to be able to brush or wash one’s hair. Sporting activity can often become difficult or impossible.
Diagnosing shoulder complaints
An x-ray of the shoulder will show the presence of arthritis. An ultrasound may be helpful in determining whether there are any other associated problems such as a tear of the tendons around the shoulder (rotator cuff), but in isolation this is a poor investigation for the diagnosis of arthritis. An MRI scan will pick up arthritis but is time consuming, expensive and usually unnecessary.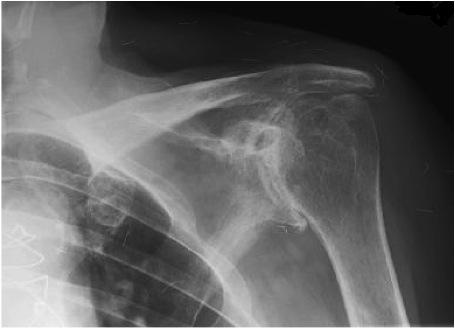
One condition that can mimic osteoarthritis with pain and stiffness is adhesive capsulitis, which is commonly called frozen shoulder. This condition is easily distinguished from osteoarthritis by x-ray however as the x-ray will be entirely normal. Frozen shoulder also occurs in a younger age group, usually affecting people in their forties.
Non-surgical treatment of shoulder problems
The first priority in management is pain control. Painkillers may be all that is required for one to cope with the pain, starting with paracetamol, and moving on to an anti-inflammatory (such as ibuprofen if there are no contraindications) and/or codeine-based analgesics. Physiotherapy is not as beneficial as it is with knee arthritis, and can sometimes make the pain worse, it is therefore not recommended.
Steroid (cortisone) injection therapy has a role in symptom control. The subacromial bursa is a pocket of fluid between the shoulder joint and the point of the shoulder, and this may become secondarily inflamed, particularly if there is an associated abnormality of the rotator cuff. However, injections into the bursa have only short-term benefits, and they will not help with stiffness. Some people advocate intra-articular steroid injections to help with the inflammation within an arthritic joint. Again effects are short-lived and it has been hypothesised that there is an increased risk to developing an infection in a prosthetic joint (shoulder replacement) when a replacement is performed after an injection.
Hyaluronan viscosupplementation injections are widely used in the knee, but again evidence shows benefits to be relatively short-lived and not very different to the results of steroid injection at six months. They again carry a small risk of infection.
Supra-scapular nerve blocks can be performed by a pain specialist to help to reduce the intensity of the pain messages coming from the shoulder and passing to the brain. This is an out-patient procedure that is performed under local anaesthetic. If the benefits are significant then it can be repeated and the sensory nerve can be ablated (irreversibly damaged) to potentially give long-term effects. This treatment option should be reserved for a patient who is unwilling to contemplate surgery, or who is at high risk of anaesthetic complications due to other serious medical conditions.
Arthroplasty or joint replacement surgery for shoulder problems
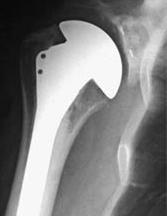
There remains much debate as to the best design of prosthesis on the market, and whether to secure the materials with or without cement. There is a choice of replacement methods on the humeral side (ball of the ball-and-socket joint) ranging from resurfacing the ball only, cutting the ball away and replacing with a very short stem, or securing a long stem down the canal of the humerus. The longest running studies report that the results of prostheses with long stems down the canal have an excellent survivorship at ten years.
More contentious is the issue of the glenoid prosthesis (socket of the ball-and-socket joint). It is technically more difficult to resurface the glenoid, and the rates of loosening are much greater than for the humeral stem. Results of resurfacing just the humeral stem are good on their own and in some patients it is not feasible to resurface the glenoid due to lack of solid supporting bone to which the prosthesis can be attached. Yet the best functional results and pain relief are when both sides of the joint are replaced. This is the ‘gold-standard.'
What special circumstances affect shoulder replacement surgery?
The shoulder joint is a very shallow ball-and-socket joint that consequently relies upon the tendons and muscles to keep the ball in the centre of the socket. When the rotator cuff is irreparably torn, the results of standard shoulder arthroplasty are not as good with regards to function and pain relief. Resurfacing of the glenoid leads to premature loosening and is therefore not performed.
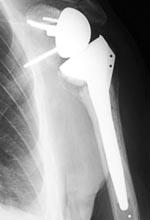
In this situation one can either insert a humeral stem with a large head or a reversed geometry prosthesis where the ball is on the side of the socket and vice versa. The latter has the advantage of altering the biomechanical environment so that the deltoid muscle can take over some of the action of the absent rotator cuff, and functional results can be excellent. Unfortunately published results of the reversed prosthesis show an increased risk of operative complications than standard shoulder arthroplasty, but this is a sub-group of patients who do worse, with or without intervention, than patients with an intact rotator cuff.
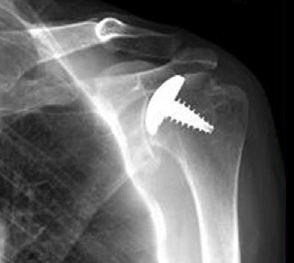
Contact sports in the modern professional era, such as rugby, have seen an increase in the physicality around the contact area, and an increased number of injuries involving the shoulder. Recurrent injuries, such as dislocations, may lead to damage to the cartilage within the gleno-humeral joint leading to early onset arthritis.
Conservative measures as described above can be adopted. For cartilage defects however, more formal surgical measures may need to be adopted. Simple surgical options include debridement of uneven areas using keyhole surgery (arthroscopic debridement) and drilling the defect to encourage healing with new cartilage (microfracture). There are more formal open operations available such as implanting cartilage cells grown in a laboratory into the defect (autologous chondrocyte implantation). This involves one operation to harvest cartilage cells from a healthy area of the body such as the knee, and a second operation to implant the new cultured cells into the defect. The final option available is arthroplasty which can just involve the limited defect, and not have to involve replacing the whole joint.
The shoulder can also be affected by avascular necrosis. This is when part of the bone involved in supporting the cartilage of the joint dies due to loss of blood supply. There are multiple causes for such a situation, but the most common is a course of high dose steroids taken for another illness such as an inflammatory condition, an HIV-related illness or spinal cord compression.
If the humeral head is affected the patient will experience pain and possibly reduction in range of movement. As the head is usually the only part of the joint affected, surgery to resurface the humerus is adequate.





